Introduction
The intricate world of pharmaceuticals extends beyond active ingredients, as excipients play a pivotal role in formulating effective medications. These inert substances not only enhance the stability and bioavailability of active pharmaceutical ingredients (APIs) but also ensure that medications remain safe and acceptable for patients. With the market for these additives continuing to grow, understanding their functions and characteristics becomes increasingly vital.
What challenges arise in the selection and application of excipients?
How do they influence the overall success of drug development?
Define Excipients: Role and Function in Drug Formulation
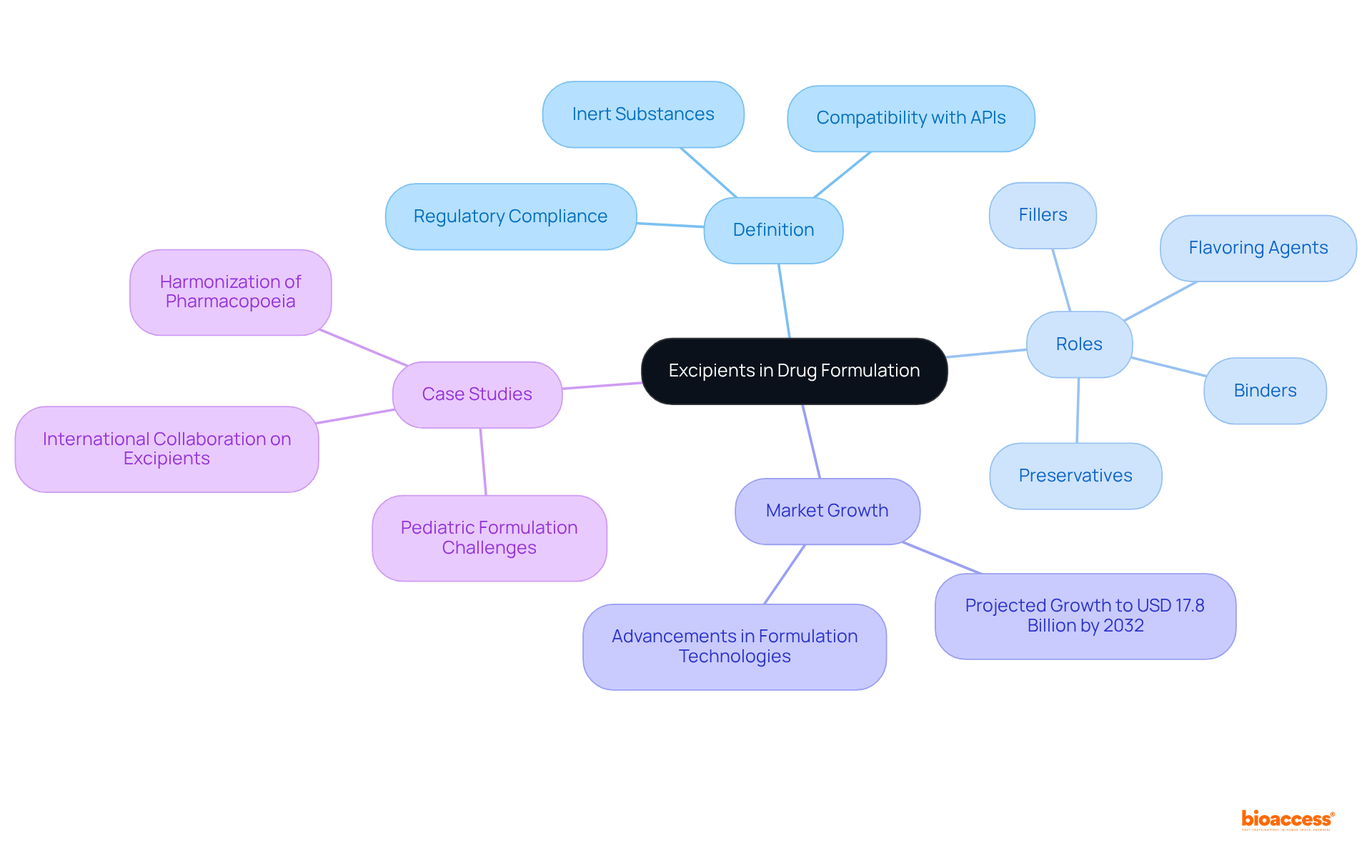
The describes inert substances that are integrated into medication mixtures, playing critical roles in the production process and of . They fulfill various functions—acting as binders, fillers, preservatives, and flavoring agents—which collectively contribute to the medication’s effectiveness, safety, and acceptability among patients. The selection of these additives is paramount; according to the , they must demonstrate compatibility with the API and comply with rigorous .
In 2025, the is underscored by their projected market growth, anticipated to reach , driven by advancements in . This expansion highlights the increasing recognition of the significant impact that have on formulation stability and bioavailability, as outlined in the , ensuring that medications maintain their integrity over time and deliver therapeutic effects efficiently. For example, multifunctional additives improve flowability and compressibility, thereby streamlining the manufacturing process while enhancing the bioavailability of APIs.
Case studies illustrate the pivotal role of additives in medication formulations. In , the meticulous selection of additives is essential due to the unique physiological differences observed in children. Research underscores the need for a clearer and quantitative data regarding additives to ensure their safe application in vulnerable populations. Moreover, the development of specialized substances has been shown to enhance the stability and sustained release of APIs, addressing formulation challenges and improving patient outcomes. As the field of drug development evolves, the role of additives will remain fundamental in ensuring the effectiveness and safety of therapeutic interventions.
Trace the History: Evolution of Excipients in Pharmaceuticals
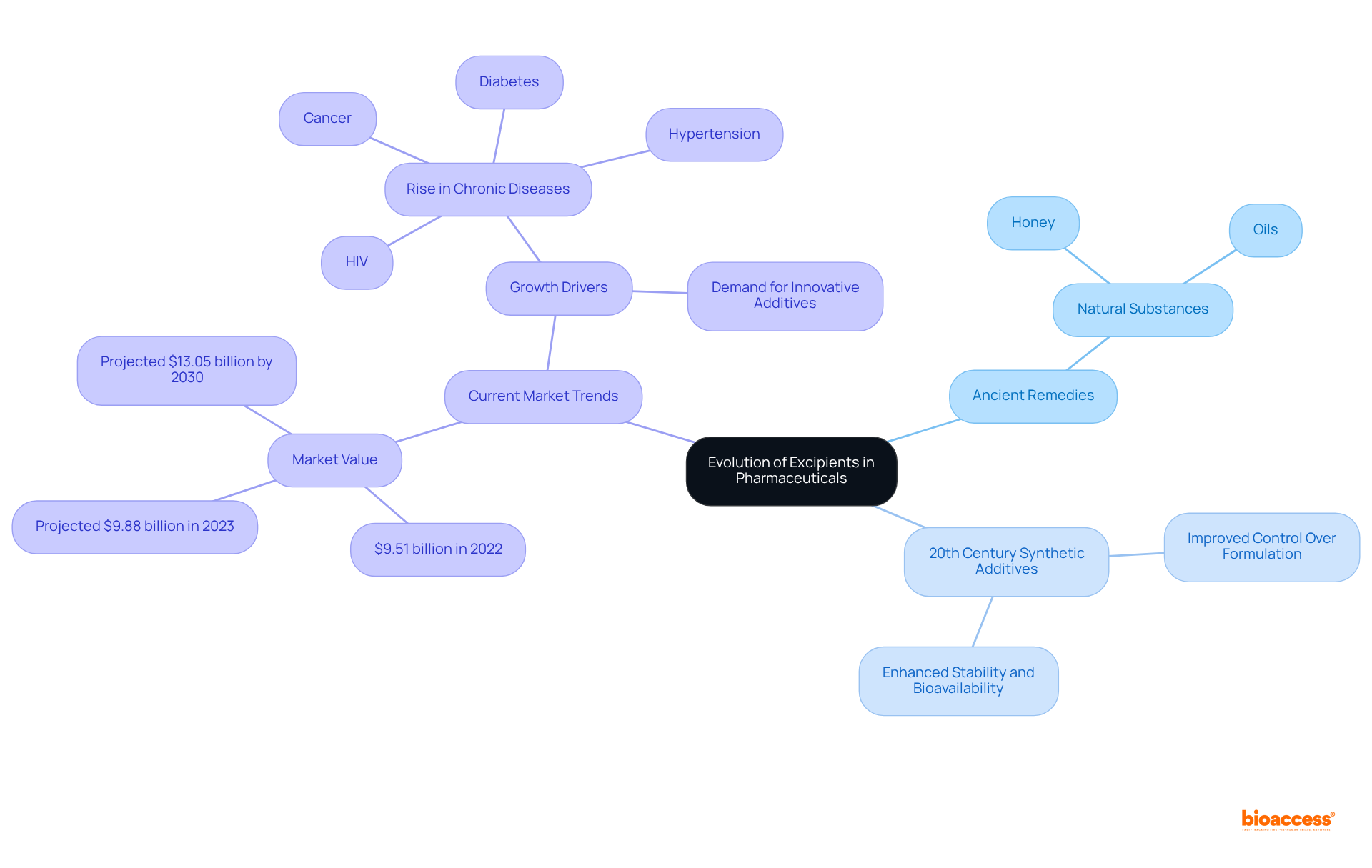
The history of dates back to ancient remedies, where natural substances such as honey and oils were utilized to enhance the delivery of . As progressed, the evolved considerably, highlighting the increasing complexity and functionality of inactive ingredients. The 20th century marked a pivotal transformation with the advent of synthetic additives, enabling improved control over formulation processes, which in turn led to . Today, the recognizes additives as rather than mere inactive fillers; they play a crucial role in influencing the of medications.
The global additives market was valued at approximately $9.51 billion in 2022 and is projected to reach $9.88 billion in 2023, reflecting a compound annual growth rate (CAGR) of 4.03% from 2023 to 2030. This growth underscores the increasing demand for , driven by the rise in chronic illnesses and the need for sophisticated medication formulations. This evolution underscores the importance of additives in enhancing and patient adherence, representing a significant advancement in medication development.
Identify Key Characteristics: Essential Properties of Excipients
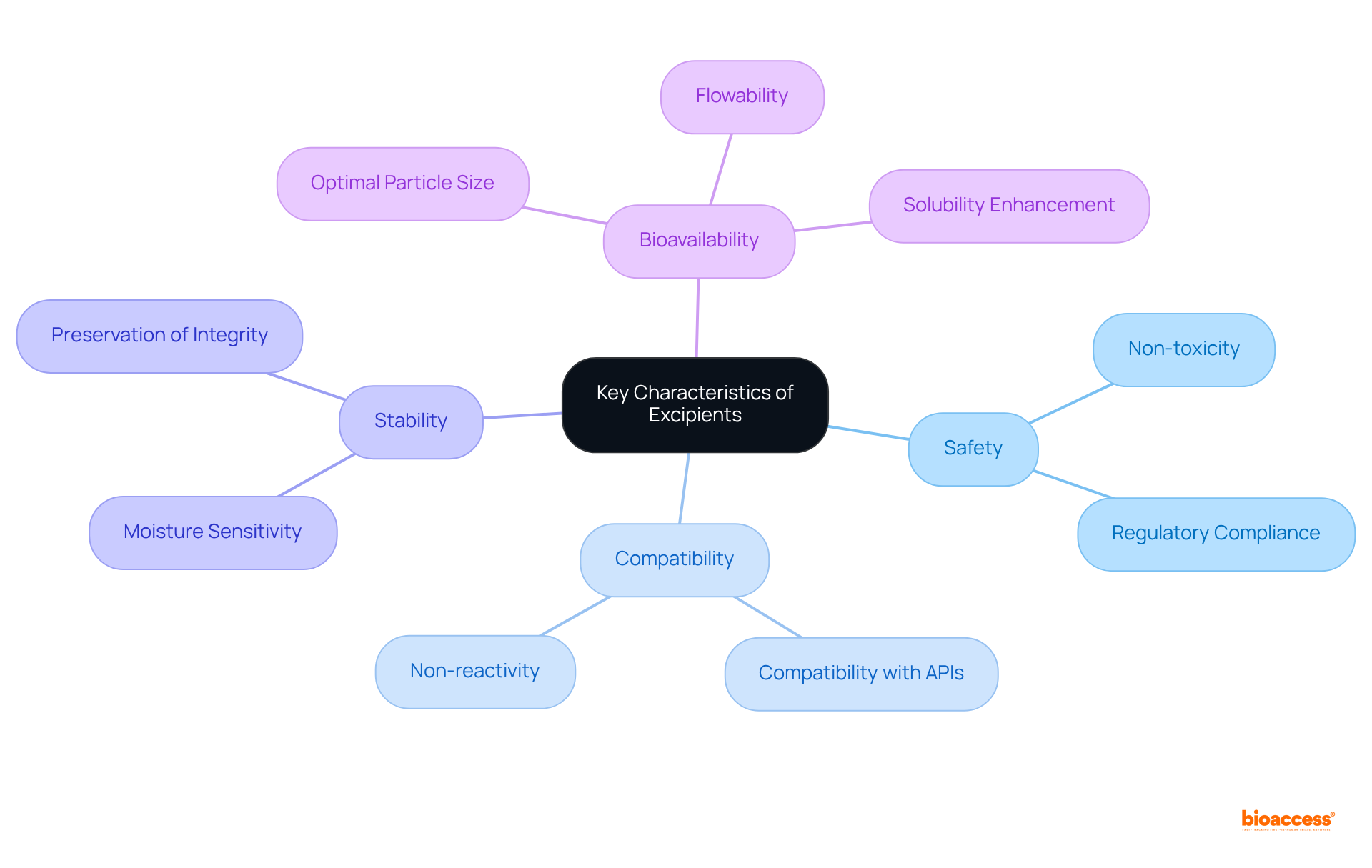
The illustrates their crucial role in formulation, characterized by their safety, compatibility with , and ability to enhance stability and bioavailability. of include non-toxicity, non-reactivity, and purity, which are critical for maintaining .
Furthermore, additives must demonstrate favorable physical characteristics such as optimal particle size, flowability, and moisture content to enable consistent manufacturing processes. For instance, lubricants like magnesium stearate are commonly employed to enhance powder flow during tablet compression, while stabilizers such as silica gel are essential for preserving the integrity of moisture-sensitive formulations.
In 2023, the demand for has surged, with the fillers and diluents segment accounting for the highest revenue share in the market. The global was valued at around 8 billion U.S. dollars, reflecting the industry’s focus on developing high-quality pharmaceuticals.
Moreover, the FDA’s endorsement of 59 innovative medications in 2023 highlights the importance of additives in new medication development. As the market evolves, adherence to stringent safety standards for additives remains paramount, ensuring that they meet and contribute positively to therapeutic outcomes.
Understand Importance: Impact of Excipients on Drug Development
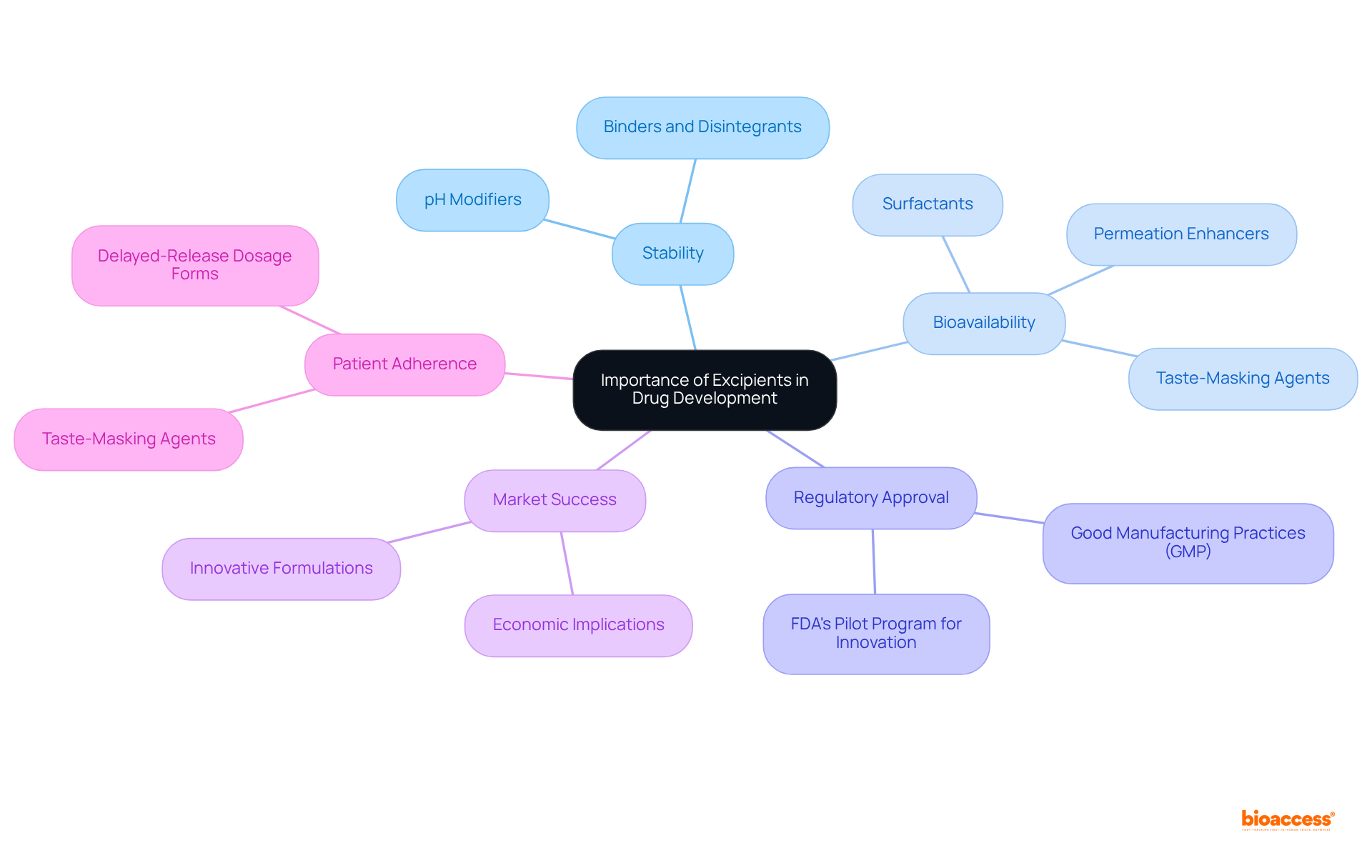
The is fundamental to medication development, as they influence not only the stability and bioavailability of formulations but also their and market success. The careful selection of additives can significantly impact the release characteristics of medications, , and overall . For example, taste-masking agents in pediatric formulations can greatly improve patient compliance with medication regimens. Moreover, as regulatory agencies intensify their scrutiny of excipient safety and functionality, understanding the becomes crucial for the successful selection of and commercialization.
Conclusion
The exploration of excipients reveals their indispensable role in drug formulation, serving as the backbone that enhances the stability, bioavailability, and overall efficacy of medications. Understanding the definition of excipients is crucial, as these inert substances are not merely fillers but vital components that ensure the safety and effectiveness of active pharmaceutical ingredients (APIs). Their significance extends beyond manufacturing, impacting patient compliance and therapeutic outcomes.
Key insights throughout the article highlight the multifaceted functions of excipients, including their historical evolution from ancient remedies to modern synthetic additives. The importance of selecting compatible and high-quality excipients is underscored, with market trends indicating a growing demand for innovative additives that cater to the complexities of contemporary drug development. Additionally, the discussion emphasizes the regulatory landscape that governs excipient usage, ensuring safety and efficacy in pharmaceutical products.
Ultimately, the significance of excipients in drug formulation cannot be overstated. As the pharmaceutical industry continues to evolve, a deeper understanding of excipients will be vital for researchers, manufacturers, and regulatory bodies alike. Embracing the complexities of excipients will lead to improved medication formulations, fostering better health outcomes and enhancing patient adherence. The call to action is clear: prioritize the study and application of excipients to unlock their full potential in the realm of pharmaceuticals.
Frequently Asked Questions
What are excipients in drug formulation?
Excipients are inert substances integrated into medication mixtures that play critical roles in the production process and enhance the stability and bioavailability of active ingredients (APIs).
What functions do excipients serve in medications?
Excipients serve various functions, including acting as binders, fillers, preservatives, and flavoring agents, which contribute to the medication’s effectiveness, safety, and patient acceptability.
Why is the selection of excipients important?
The selection of excipients is crucial because they must demonstrate compatibility with the API and comply with rigorous regulatory standards for safety and efficacy.
What is the projected market growth for excipients by 2032?
The market for excipients is projected to reach USD 17.8 billion by 2032, driven by advancements in formulation technologies.
How do multifunctional additives impact drug formulation?
Multifunctional additives improve flowability and compressibility, streamlining the manufacturing process while enhancing the bioavailability of APIs.
Why is the selection of additives critical in pediatric preparations?
The selection of additives is essential in pediatric preparations due to the unique physiological differences in children, necessitating careful consideration to ensure safety.
What challenges do specialized substances address in drug formulation?
Specialized substances enhance the stability and sustained release of APIs, addressing formulation challenges and improving patient outcomes.
What is the significance of excipients in the evolving field of drug development?
As drug development evolves, the role of excipients remains fundamental in ensuring the effectiveness and safety of therapeutic interventions.
List of Sources
- Define Excipients: Role and Function in Drug Formulation
- statista.com (https://statista.com/topics/12873/active-pharmaceutical-ingredients-apis-and-excipients)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9026161)
- snsinsider.com (https://snsinsider.com/reports/pharmaceutical-excipients-market-2584)
- biospace.com (https://biospace.com/press-releases/pharmaceutical-excipients-market-size-worth-usd-15-6-billion-by-2034-driven-by-demand-for-advanced-drug-delivery-and-rising-chronic-disease)
- futuredatastats.com (https://futuredatastats.com/excipients-market?srsltid=AfmBOoq6P4cN7gTHdiN3bsKY9MK7XfktOTU_71gR76IcSrlrT8ynld7i)
- Trace the History: Evolution of Excipients in Pharmaceuticals
- bccresearch.com (https://bccresearch.com/market-research/pharmaceuticals/excipients-in-pharmaceuticals-global-markets.html?srsltid=AfmBOoqci0cIBcvEY7AJqvkbQgx9xjiWZiaqYsaYf5W2W4Boo350IT_3)
- grandviewresearch.com (https://grandviewresearch.com/industry-analysis/excipients-market-analysis)
- futuredatastats.com (https://futuredatastats.com/pharmaceutical-excipients-market?srsltid=AfmBOoqkl19BNATdeN0r4yoB1h2fsZqxz9fKo-pbpcs9igHJGZH-YVyJ)
- statista.com (https://statista.com/statistics/1496725/pharmaceutical-excipients-market-share-worldwide-by-region)
- biospace.com (https://biospace.com/press-releases/pharmaceutical-excipients-market-size-worth-usd-15-6-billion-by-2034-driven-by-demand-for-advanced-drug-delivery-and-rising-chronic-disease)
- Identify Key Characteristics: Essential Properties of Excipients
- statista.com (https://statista.com/statistics/1497288/leading-excipients-in-biotech-drugs)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9010397)
- pharmamanufacturing.com (https://pharmamanufacturing.com/sector/large-molecule/article/11311231/trends-in-excipient-demand)
- snsinsider.com (https://snsinsider.com/reports/pharmaceutical-excipients-market-2584)
- statista.com (https://statista.com/topics/12873/active-pharmaceutical-ingredients-apis-and-excipients)
- Understand Importance: Impact of Excipients on Drug Development
- drugpatentwatch.com (https://drugpatentwatch.com/blog/grow-your-excipient-business-by-tracking-drug-patents?srsltid=AfmBOorsJN6eKiRclON4_XvohjD8uhoLNxkyti13pmEK7lfFlNQhbsga)
- snsinsider.com (https://snsinsider.com/reports/pharmaceutical-excipients-market-2584)
- drugpatentwatch.com (https://drugpatentwatch.com/blog/how-excipients-shape-drug-effectiveness?srsltid=AfmBOoqL8ImVuDucoUysGsRJflvQUD_p50ZhCpMufTJMy4Zu3VKlmxtG)
- biospace.com (https://biospace.com/press-releases/pharmaceutical-excipients-market-size-worth-usd-15-6-billion-by-2034-driven-by-demand-for-advanced-drug-delivery-and-rising-chronic-disease)


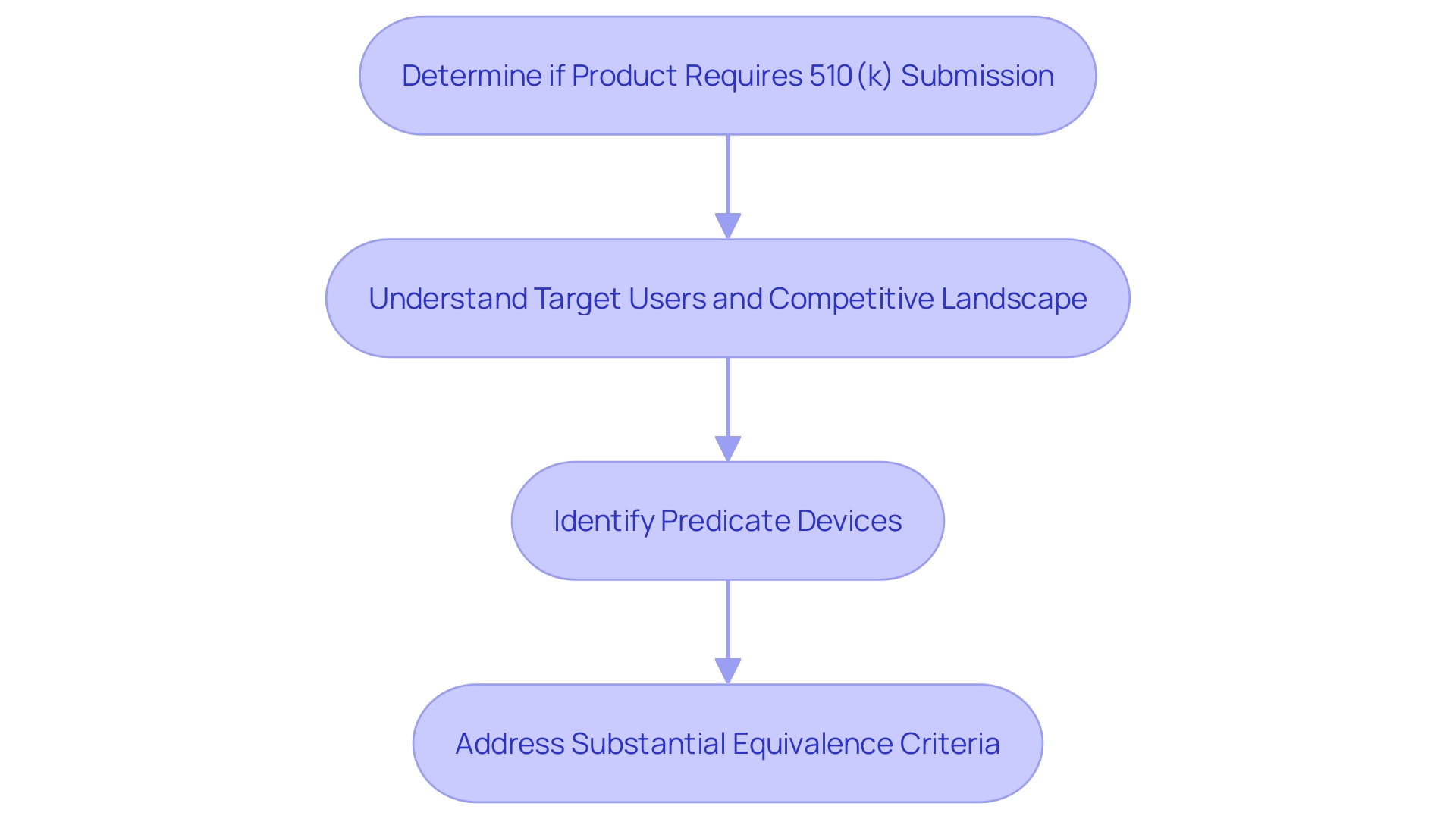
 for a 510(k) submission, highlighting the key steps and considerations involved. This flowchart illustrates the process of identifying a suitable predicate product for a 510(k) submission, highlighting the key steps and considerations involved.](https://tely.blob.core.windows.net/telyai/this-flowchart-illustrates-the-process-of-identifying-a-suitable-predicate-product-for-a-510-k-submission-highlighting-the-key-steps-and-considerations-involved.jpg)