Introduction
Understanding the nuances between precision and accuracy is vital in the realm of clinical research, where the stakes are high and the implications of data can affect patient care. This article delves into the critical differences between these two concepts, shedding light on their significance in ensuring reliable research outcomes. With nearly 30% of medical studies failing due to information-related issues, the question arises: how can researchers effectively enhance both precision and accuracy to safeguard the integrity of their findings?
Define Accuracy and Precision in Clinical Research
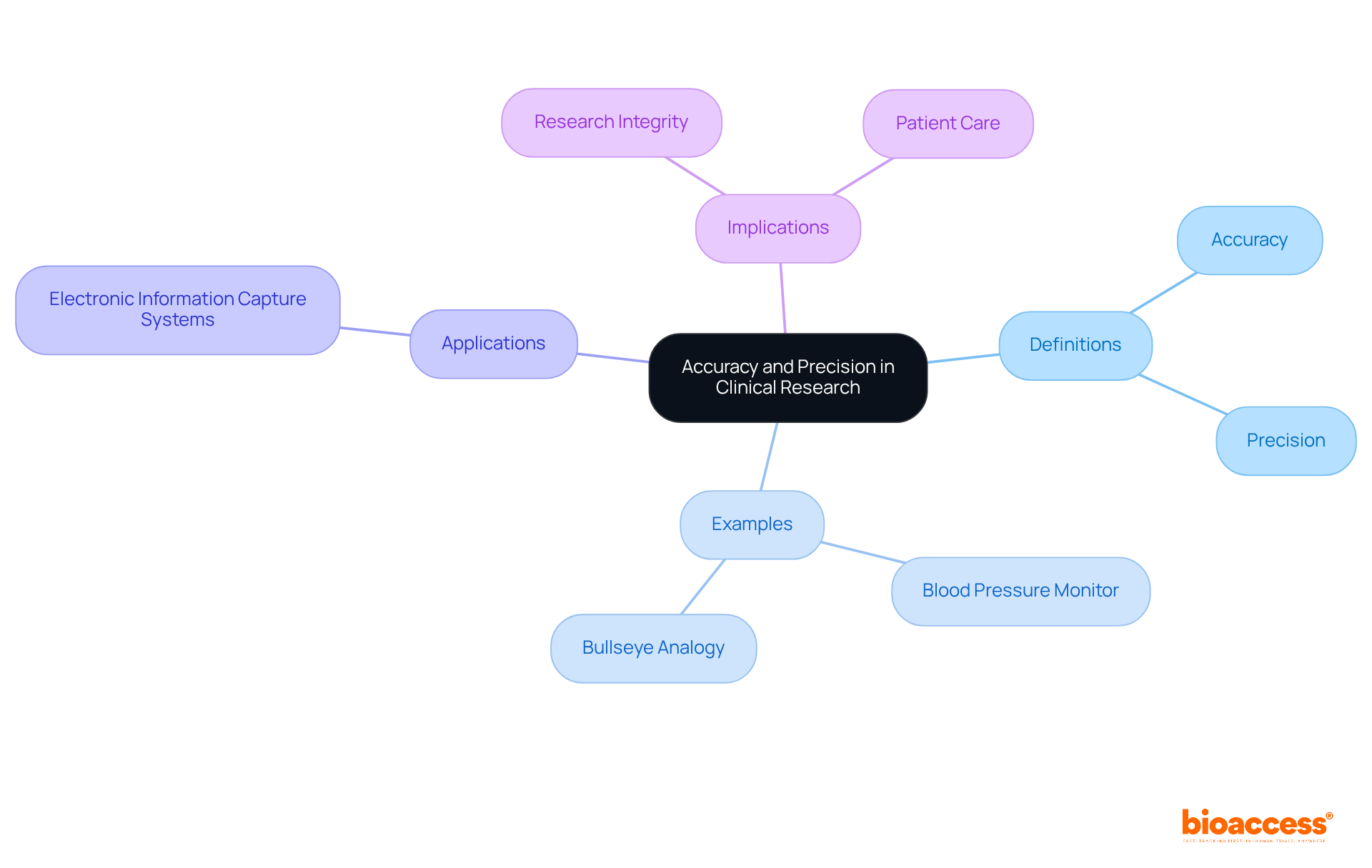
In medical research, . For instance, a blood pressure monitor that consistently displays a reading of 120/80 mmHg when the actual pressure is indeed 120/80 mmHg is considered accurate. Conversely, accuracy also pertains to the . If the same blood pressure monitor yields readings of 120/80 mmHg multiple times, it is deemed precise, regardless of whether those readings are accurate.
This differentiation is crucial, as it is important to explain the to avoid threatening the integrity of research results. A study revealed that nearly 30% of due to information-related problems, underscoring the .
Practical applications, such as the use of electronic information capture systems, have demonstrated a reduction in entry mistakes by up to 50%, significantly improving both in research trials. Understanding these concepts is essential to explain the , as it aids in interpreting data correctly and ensures the , ultimately contributing to improved patient care.
To illustrate, consider the bullseye analogy: accurate results land close to the bullseye, while precise results cluster closely together. Furthermore, utilizing calibrated tools reduces measurement errors, highlighting the significance of in research.
Discuss the Importance of Accuracy and Precision in Clinical Trials
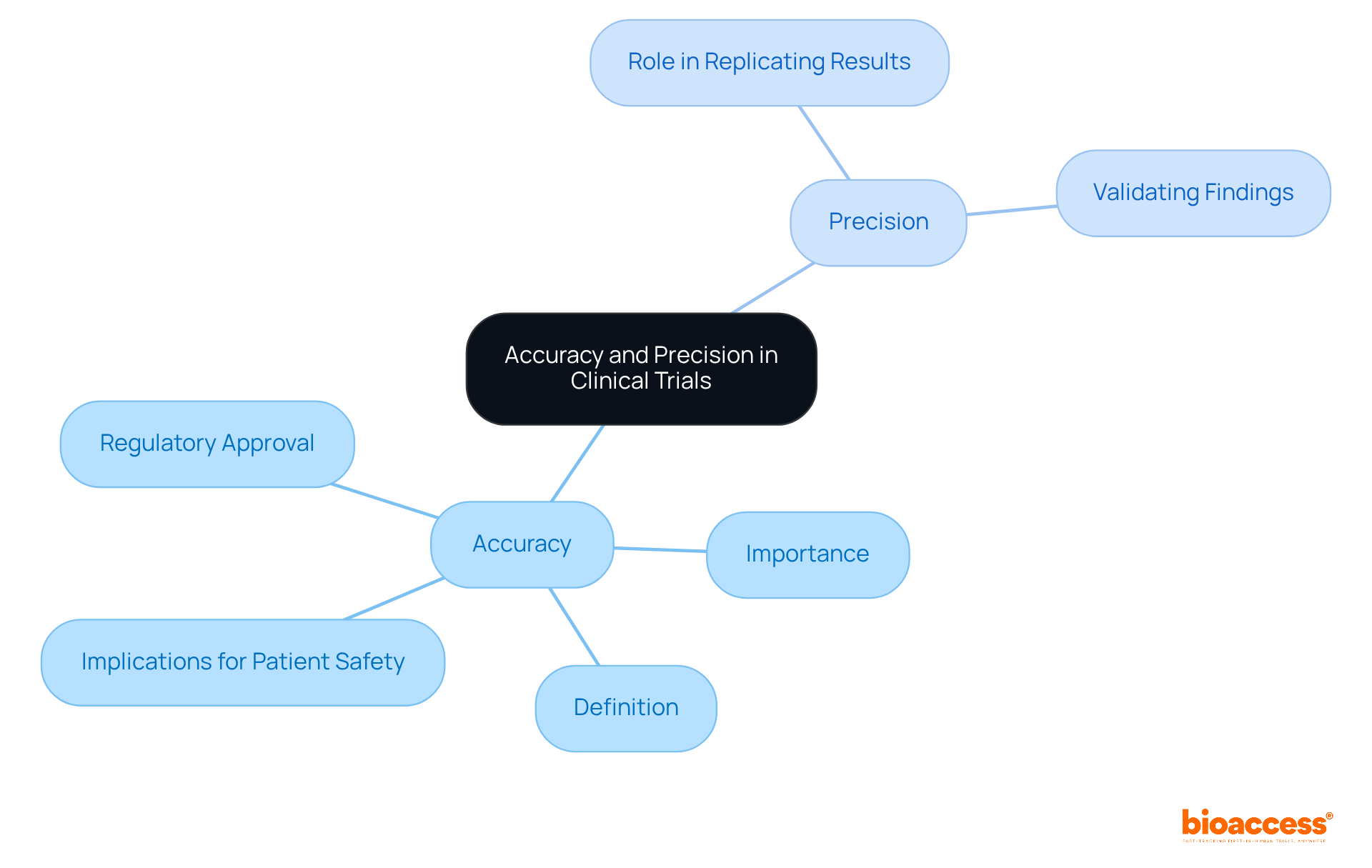
In research trials, it is crucial to explain the , as both are paramount in underpinning the reliability of trial outcomes. Precise information ensures that the results reflect the true effectiveness and safety of a treatment, a critical factor for and informed . Furthermore, precision enables researchers to replicate results consistently, which is essential for validating findings.
It is essential to explain the , as inaccurate or imprecise data can lead to , regulatory setbacks, and even patient harm. Therefore, upholding is vital for the success of .
Implement Strategies to Measure and Enhance Accuracy and Precision
To enhance in clinical research, particularly in the context of medical device , it is essential to implement the following strategies:
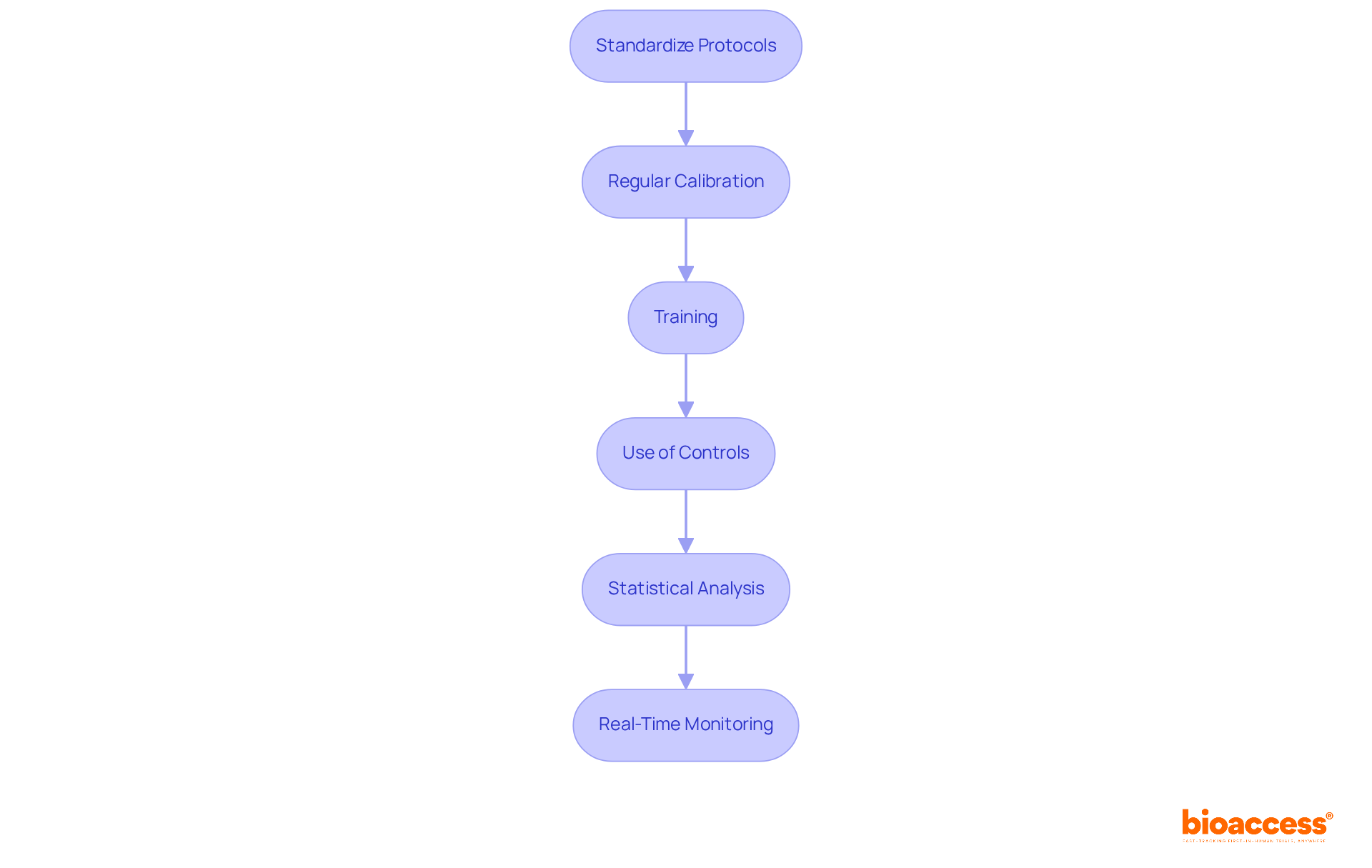
- Standardize Protocols: Establish clear and consistent protocols for data collection and evaluation. This minimizes variability and improves both , which is vital in studies such as Early-Feasibility and that aim to explain the difference between precision and accuracy.
- Regular Calibration: Ensure that all measuring instruments are consistently calibrated and maintained to prevent systematic errors. This practice is highlighted in thorough management services for studies.
- Training: Provide comprehensive instruction for all personnel involved in information collection to minimize human error. Tailored training programs are essential to ensure that teams are well-prepared for the complexities of .
- Use of Controls: Implement control measures to monitor the accuracy of information collection methods, which is essential in .
- Statistical Analysis: Employ appropriate to analyze information, helping to identify outliers and assess the reliability of measurements. This is a key component of effective reporting processes.
- Real-Time Monitoring: Utilize systems to catch errors as they occur, allowing for immediate corrective actions and enhancing the efficiency of Post-Market Clinical Follow-Up Studies (PMCF).
Troubleshoot Common Issues with Accuracy and Precision in Clinical Research
Common issues affecting accuracy and precision in include:
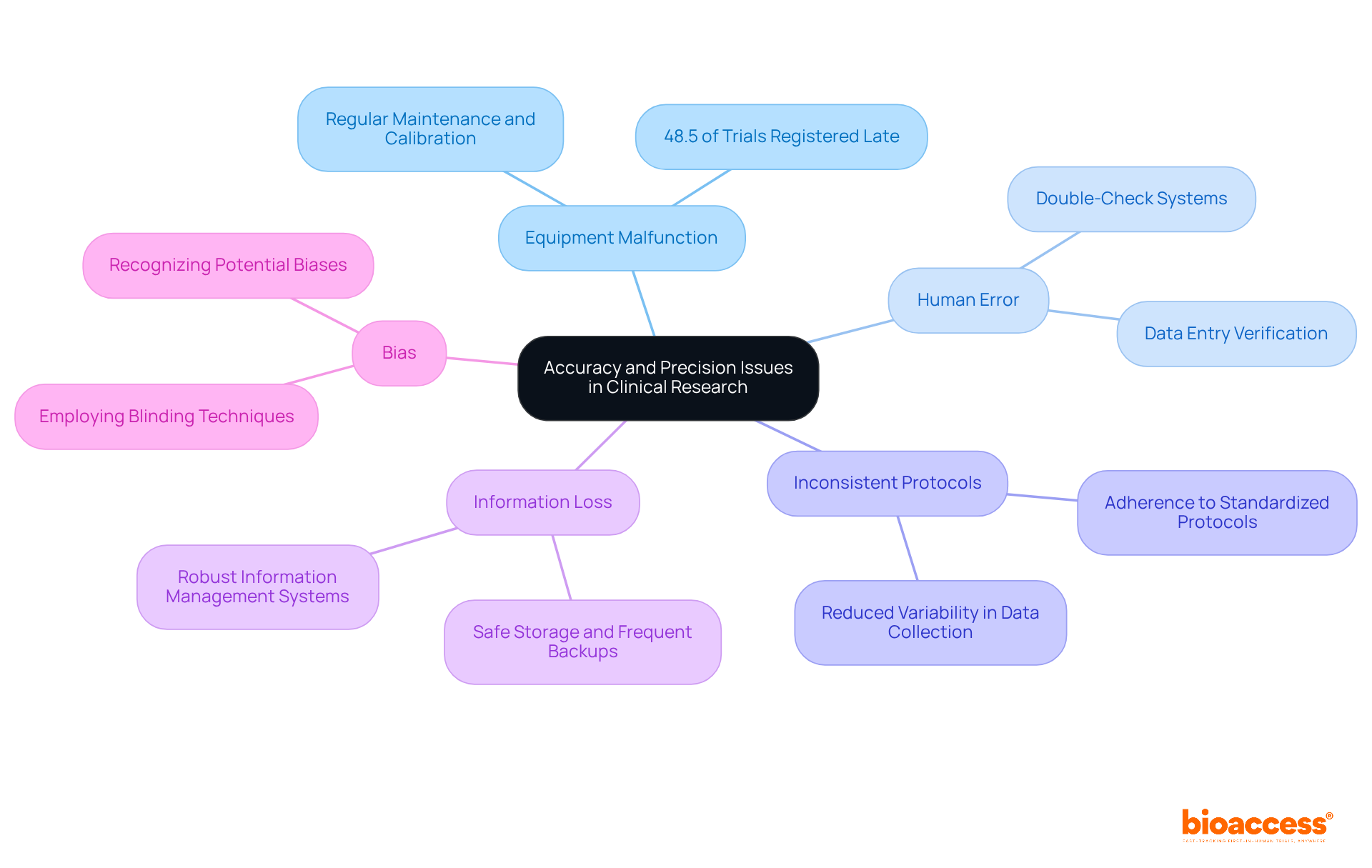
- Equipment Malfunction: Regular maintenance and calibration of equipment are essential to prevent malfunctions that can compromise measurement accuracy. Statistics reveal that significantly contribute to inaccuracies, with malfunction rates adversely affecting test results. Notably, 48.5% of were registered late, underscoring the necessity for timely equipment checks.
- Human Error: Implementing is crucial. Data entry and measurements should be verified by multiple personnel to minimize the risk of errors that can skew results.
- Inconsistent Protocols: Adherence to is vital. Ensuring that all team members follow the same procedures reduces variability in information collection, which can lead to discrepancies in outcomes.
- Information Loss: Robust are essential to prevent information loss. Safe storage and frequent backups of gathered data guarantee that valuable details are preserved, which is critical for maintaining the integrity of clinical studies.
- Bias: and analysis is essential. Employing blinding techniques can help mitigate the effects of bias, ensuring that results are more reliable and reflective of true outcomes.
A notable case study illustrated that misreported patient responses led to a trial’s termination and a loss of investor confidence, highlighting the critical importance of addressing these common issues. As Thomas Redman remarked, “Where there is data smoke, there is business fire,” emphasizing the necessity of ensuring accuracy and exactness in medical research. By addressing these common issues, teams can explain the difference between precision and accuracy, enhancing the overall reliability of their studies and ultimately improving patient safety.
Conclusion
Understanding the distinction between precision and accuracy is essential for achieving reliable outcomes in clinical research. These concepts extend beyond academic theory; they hold significant implications that directly impact patient care and the credibility of medical studies. Mastering the nuances of accuracy and precision empowers researchers to enhance the integrity of their findings and drive advancements in healthcare.
This article outlines several key points, emphasizing:
- The necessity of standardized protocols
- Regular calibration of instruments
- Comprehensive training for personnel involved in data collection
It highlights the detrimental effects of inaccuracies and imprecisions, which can lead to flawed conclusions, regulatory challenges, and potential harm to patients. Strategies such as real-time monitoring and rigorous statistical analysis further reinforce the imperative of maintaining high standards in clinical trials.
Ultimately, the message is clear: prioritizing accuracy and precision is not merely a best practice; it is a fundamental requirement for successful clinical research. Researchers must adopt strategies that enhance these qualities, ensuring their studies yield trustworthy data. By doing so, they not only protect the integrity of their research but also uphold the safety and well-being of patients, paving the way for more effective treatments and improved healthcare outcomes.
Frequently Asked Questions
What is the definition of accuracy in clinical research?
Accuracy in clinical research is defined as the degree to which a measured value corresponds to the true or accepted value.
What does precision mean in the context of clinical research?
Precision refers to the consistency of repeated measurements. A measurement is considered precise if it yields the same result multiple times, regardless of whether those results are accurate.
Why is it important to differentiate between accuracy and precision in research?
Differentiating between accuracy and precision is crucial to avoid compromising the integrity of research results. Misunderstanding these concepts can lead to significant information-related problems in studies.
What percentage of medical studies fail due to information-related problems?
Nearly 30% of medical studies fail due to information-related problems.
How can electronic information capture systems improve accuracy and precision in research trials?
The use of electronic information capture systems has been shown to reduce entry mistakes by up to 50%, significantly enhancing both accuracy and precision in research trials.
How can the bullseye analogy help in understanding accuracy and precision?
The bullseye analogy illustrates that accurate results are those that land close to the bullseye (true value), while precise results are those that cluster closely together, indicating consistency.
What role do calibrated tools play in ensuring accuracy and precision in research?
Utilizing calibrated tools helps reduce measurement errors, highlighting the significance of maintaining both accuracy and precision in research.
List of Sources
- Define Accuracy and Precision in Clinical Research
- asana.com (https://asana.com/resources/accuracy-vs-precision)
- bioaccessla.com (https://bioaccessla.com/blog/7-key-differences-between-accurately-vs-precisely-in-clinical-research)
- Troubleshoot Common Issues with Accuracy and Precision in Clinical Research
- bioaccessla.com (https://bioaccessla.com/blog/7-key-differences-between-accurately-vs-precisely-in-clinical-research)
- Accuracy vs. Precision vs. Reliability (https://accuracyresearch.com/blog/accuracy-vs-precision-vs-reliability)

Leave a Reply