Introduction
As the landscape of chronic kidney disease (CKD) management evolves, 2024 is set to unveil a range of innovative treatments that could redefine patient care. With advances spanning groundbreaking medications and cutting-edge diagnostic tools, these developments have the potential to significantly enhance patient outcomes and quality of life. Yet, amidst this wave of innovation, critical questions emerge:
- How will these new treatments integrate into existing care protocols?
- What challenges must be navigated to ensure accessibility and effectiveness?
This article delves into ten transformative treatments poised to make an impact in the coming year, offering insights into their mechanisms, benefits, and the future of CKD management.
bioaccess: Accelerated Clinical Research Services for CKD Treatments
bioaccess® stands out as a , dedicated to accelerating for solutions. With a deep understanding of regulatory landscapes across Latin America, the Balkans, and Australia, bioaccess® achieves ethical approvals in an impressive 4-6 weeks and activates in under 8 weeks. This swift process not only reduces the time to market for the but also significantly improves patient access to groundbreaking therapies. Their commitment to early-phase studies guarantees that promising CKD interventions are assessed with efficiency and precision.
In addition to their rapid timelines, bioaccess® provides a comprehensive suite of services, including:
- Subject recruitment
- Trial data management
This holistic approach streamlines the , ensuring compliance and ultimately accelerating the path to commercialization. By addressing key challenges in the Medtech landscape, bioaccess® positions itself as a vital partner for those looking to navigate the complexities of clinical research.
Collaboration is essential in this field, and bioaccess® is poised to lead the way. As the demand for innovative CKD therapies increases, particularly with the anticipated , the importance of partnering with a knowledgeable CRO cannot be overstated. Engage with bioaccess® today to explore how their expertise can enhance your clinical research efforts.
Sodium-Glucose Cotransporter-2 Inhibitors: Innovative Approach to CKD Management
Sodium-glucose cotransporter-2 (SGLT2) inhibitors represent a of (CKD). These medications work by preventing glucose reabsorption in the kidneys, which not only but also alleviates renal workload, ultimately leading to improved organ function. Recent have shown that , with one study revealing a remarkable 41% reduction in the risk of major adverse renal events (MAKEs) compared to RAAS blockade. Furthermore, these medications are associated with a 48% decreased risk of progressing to CKD stage 5, indicated by a hazard ratio of 0.52, underscoring their potential to enhance .
The ; they also offer cardiovascular benefits and (AKI). However, it is crucial to remain vigilant regarding potential adverse effects, particularly urinary tract infections (UTIs), which are the most commonly reported side effects. As the evidence supporting the use of SGLT2 inhibitors continues to expand, they are solidifying their role as a cornerstone in CKD management, which may contribute to the , providing renewed hope for both patients and healthcare providers. This growing body of research not only emphasizes the but also encourages further exploration and collaboration in the field.
Cystatin C: A Key Biomarker for GFR Assessment in CKD
(GFR) in patients with . Unlike creatinine, cystatin C levels are less influenced by muscle mass, making it a more . This reliability allows for in clinical settings. As research continues to validate its effectiveness, cystatin C is poised to become a standard in , ultimately enhancing .
Point-of-Care Testing: Enhancing CKD Management Through Immediate Results
is transforming the management of (CKD) by providing immediate results for essential biomarkers, such as creatinine and electrolytes. This rapid testing capability allows healthcare professionals to make timely adjustments, significantly . For example, studies indicate that the i-STAT device can deliver results in just minutes, boasting a sensitivity of 99% for detecting creatinine levels of 1.5 mg/dL or higher. This enables clinicians to respond quickly to concerning clinical findings.
The integration of POCT into clinical practice not only facilitates better monitoring of disease progression but also promotes greater patient engagement, as individuals receive instant feedback on their health status. Furthermore, the convenience and efficiency of POCT represent a substantial advancement in managing . Evidence suggests that and improved overall support for those with CKD. As Salvatore Viscomi, M.D., pointed out, the ongoing development of these technologies is vital for addressing and intervention for CKD.
The POCT market was valued at approximately USD 44 billion in 2022 and is projected to reach USD 78 billion by 2030, highlighting the increasing importance of this technology in healthcare. With the rising prevalence of CKD, the introduction of a in 2024 highlights the ever-increasing critical role of POCT in enhancing care and optimizing management strategies. A community study in León, Nicaragua, underscores the importance of , demonstrating their effectiveness in .
Individual Risk Assessment: Tailoring CKD Treatments for Better Outcomes
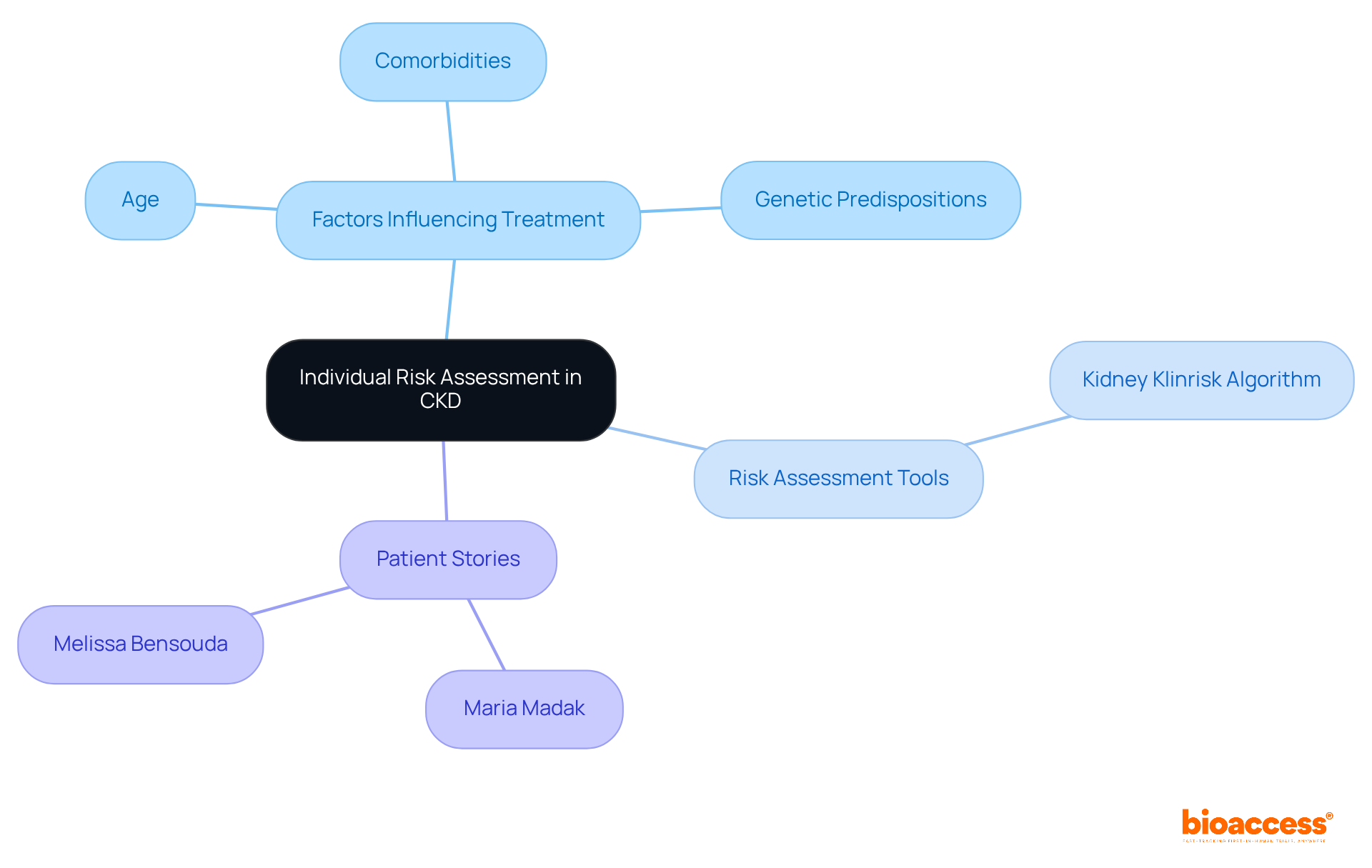
Personal risk evaluation is essential in managing (CKD), enabling to customize care based on each individual’s unique profile. Factors such as age, comorbidities, and genetic predispositions play a significant role in influencing treatment outcomes. By employing advanced risk assessment tools like the , clinicians can identify high-risk individuals and implement , leading to better management of CKD and improved outcomes.
As Maria Madak, an IgA Nephropathy patient and transplant recipient, aptly states, “For anyone who has kidney disease… have hope. Be alert, eat right, take your medications, and be persistent with your lab and doctor visits.” This is increasingly vital in modern medicine, aligning care strategies with the distinct needs of individuals and fostering a more effective .
Moreover, the success stories of individuals like Melissa Bensouda, who has thrived for over twenty years post-diagnosis, highlight the transformative potential of . By integrating , can develop a comprehensive care model that not only addresses medical needs but also empowers individuals to lead fulfilling lives.
Delaying CKD Progression: Strategies for Effective Management
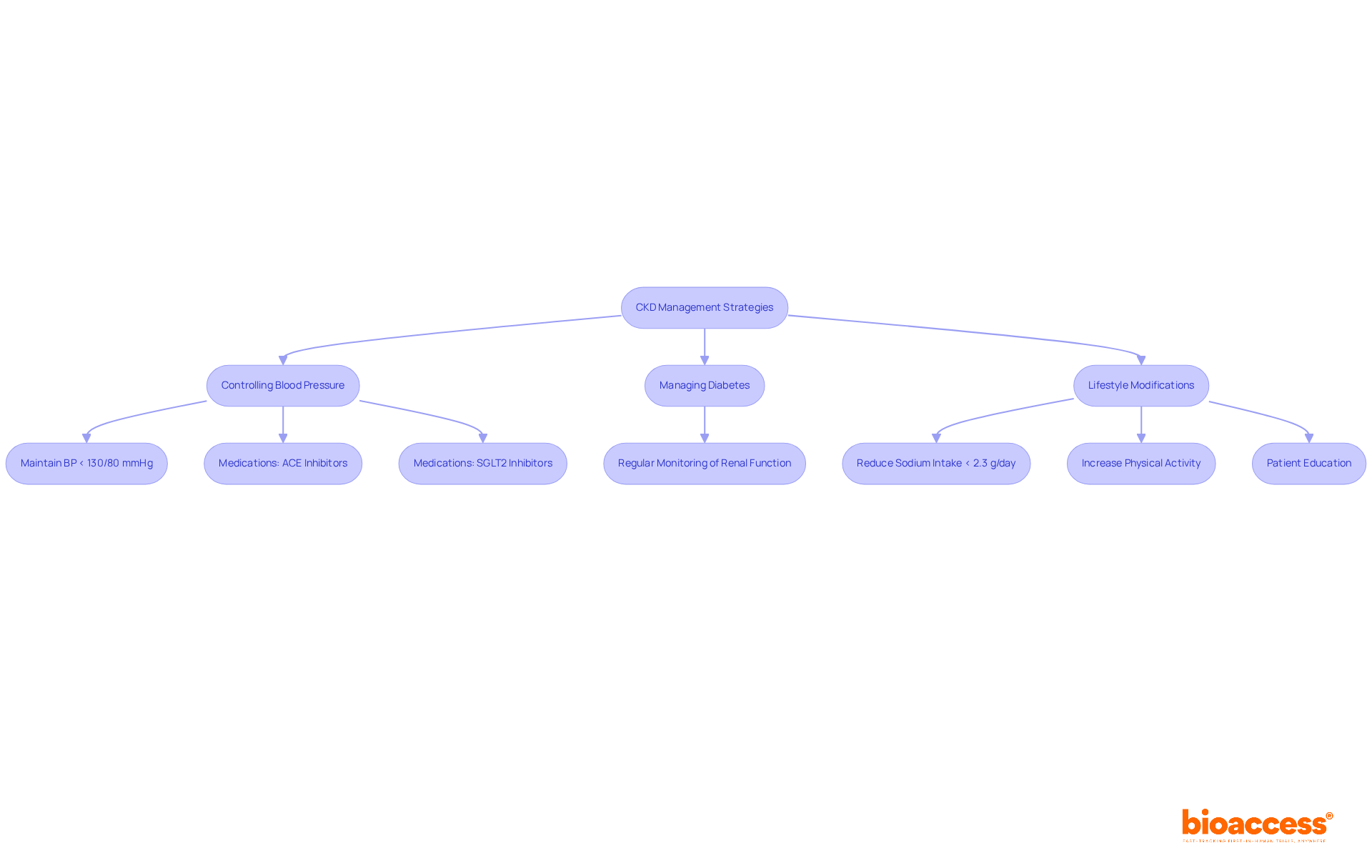
Postponing the advancement of (CKD) is crucial for improving . typically include several key strategies:
- Managing diabetes
- Implementing
For instance, keeping blood pressure below 130/80 mmHg is vital, as hypertension significantly contributes to CKD progression. Additionally, dietary changes, like reducing sodium intake to less than 2.3 g/day, can effectively lower blood pressure and decrease proteinuria, thereby slowing disease advancement. The World Health Organization endorses this as a cost-effective public health measure.
Medications such as have proven effective in delaying CKD progression. These therapies not only help manage blood pressure but also provide renal protective benefits, making them essential components of a comprehensive management strategy. , including (eGFR) and albuminuria levels, is critical for assessing treatment effectiveness and adjusting strategies as needed.
Patient education is pivotal in management, empowering individuals to embrace healthier lifestyles. Research shows that lifestyle modifications, including increased physical activity and weight management, can significantly enhance quality of life and lower the risk of CKD progression. As Akihiro Kuma noted, “Lifestyle interventions seem to positively affect some risk factors for progression of CKD and quality of life.” For example, a systematic review revealed that , including creatinine levels and blood pressure.
By focusing on these multifaceted strategies, healthcare providers can enhance the quality of life for individuals with CKD and alleviate the burden of the disease, ultimately leading to better long-term outcomes. Notably, affects 10% of adults globally, with its prevalence rising by 88% from 1990 to 2016, underscoring the urgent need for effective management strategies.
Hyperuricemia Management: Addressing a Common CKD Complication
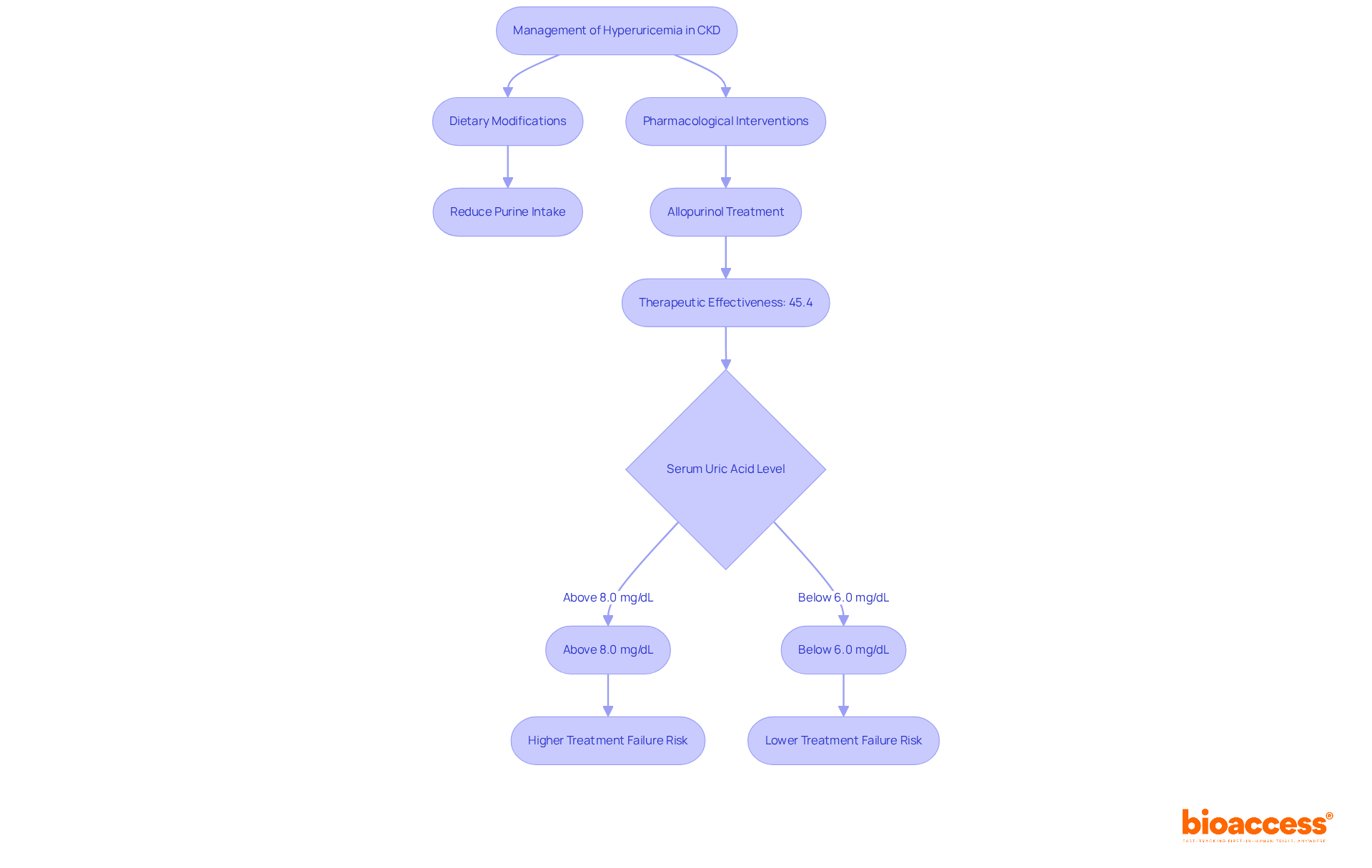
Hyperuricemia, characterized by elevated uric acid levels, is a prevalent complication in individuals with (CKD). This condition not only exacerbates renal damage but also . are essential, including:
Research shows that , achieving therapeutic effectiveness in about 45.4% of those treated. Furthermore, individuals with mean serum uric acid levels above 8.0 mg/dL face a greater likelihood of treatment failure compared to those with levels below 6.0 mg/dL. This underscores the critical need for consistent . By addressing hyperuricemia, healthcare providers can enhance renal health and improve overall well-being, emphasizing the importance of a with the new .
Statin Use: Evaluating Benefits for CKD Patients
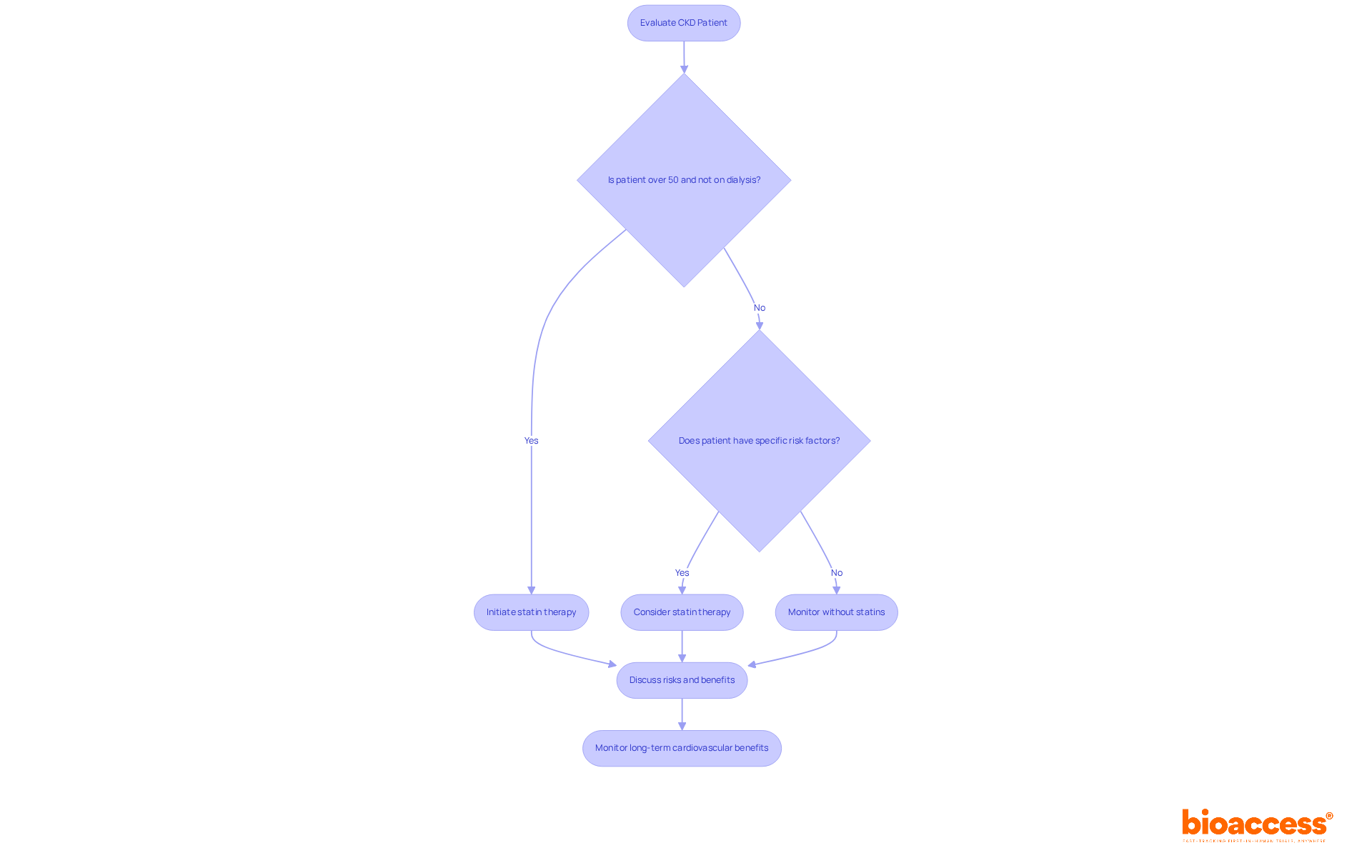
Statins are frequently recommended for individuals with to effectively manage dyslipidemia and mitigate . Research indicates that can significantly reduce the occurrence of cardiovascular events in this population, which is crucial given the heightened risk of heart disease among those with CKD. For instance, studies reveal that is associated with a 23% decrease in all-cause mortality among hyperlipidemic individuals undergoing dialysis who have a history of myocardial infarction or percutaneous coronary intervention, underscoring its potential benefits.
However, initiating requires careful customization based on , including and the risk of side effects such as muscle cramping, tenderness, and weakness, as well as liver enzyme elevation. Current guidelines advocate for statins in individuals with CKD over 50 years old who are not on dialysis, while younger individuals aged 18-49 may be considered if they exhibit . Furthermore, the KDIGO guidelines emphasize a ‘fire and forget’ approach when starting in individuals with CKD.
Ongoing research continues to investigate the in CKD management, making this a vital area for to monitor and address. It is essential for to engage in discussions about the risks and benefits of with their patients, ensuring informed decision-making.
New Experimental Treatments: Exploring Innovations in CKD Care
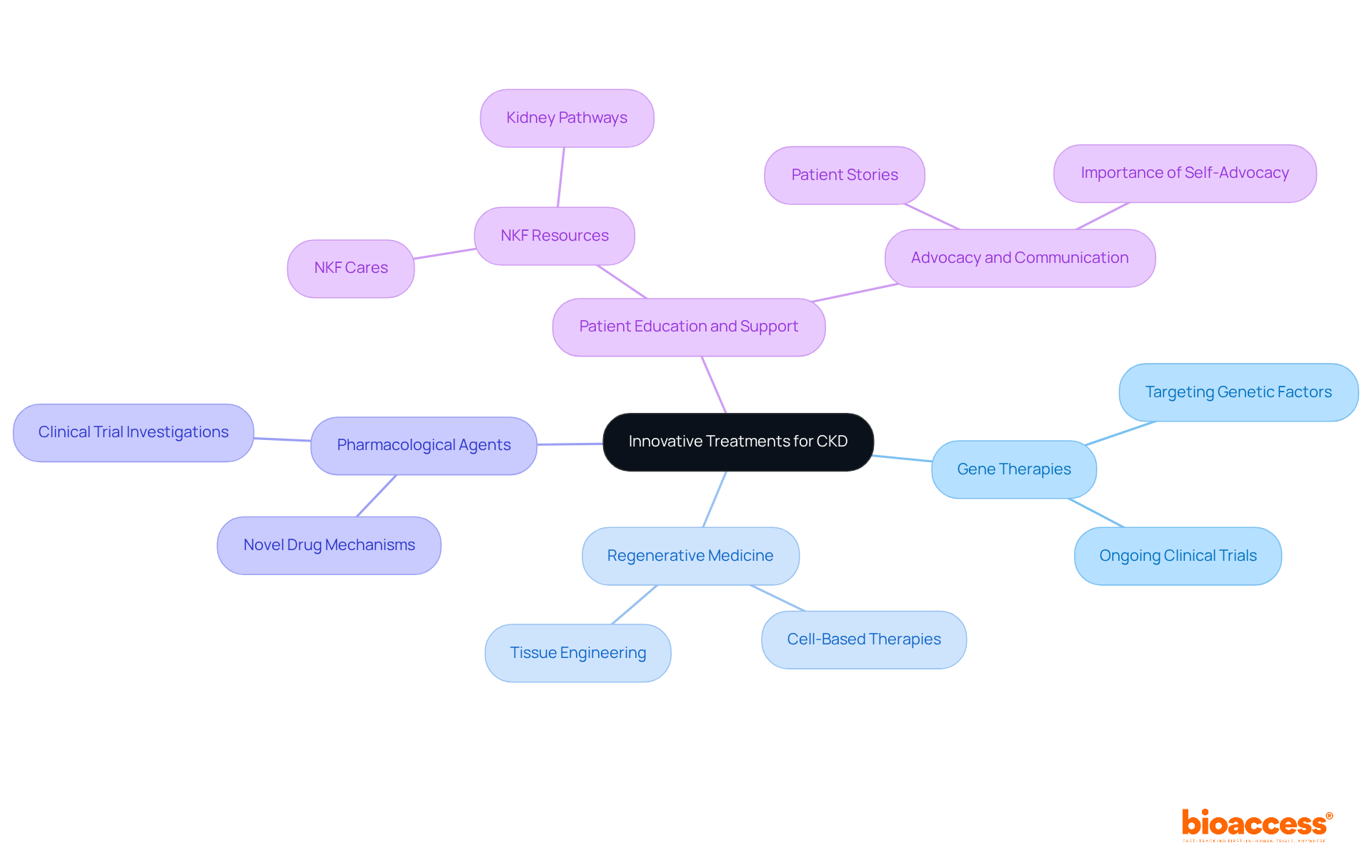
are emerging for (CKD), including a , driven by extensive research into , , and novel pharmacological agents that specifically target pathways of kidney damage. Ongoing are investigating these therapies as a , which hold the potential to and instill .
For instance, are currently being tested in , aiming to tackle the underlying genetic factors that contribute to CKD progression. As these advancements unfold, it is essential for healthcare providers to stay updated on the , particularly the , ensuring they can deliver the most effective care to those grappling with this challenging condition.
Clinical Trials: Paving the Way for New CKD Treatments
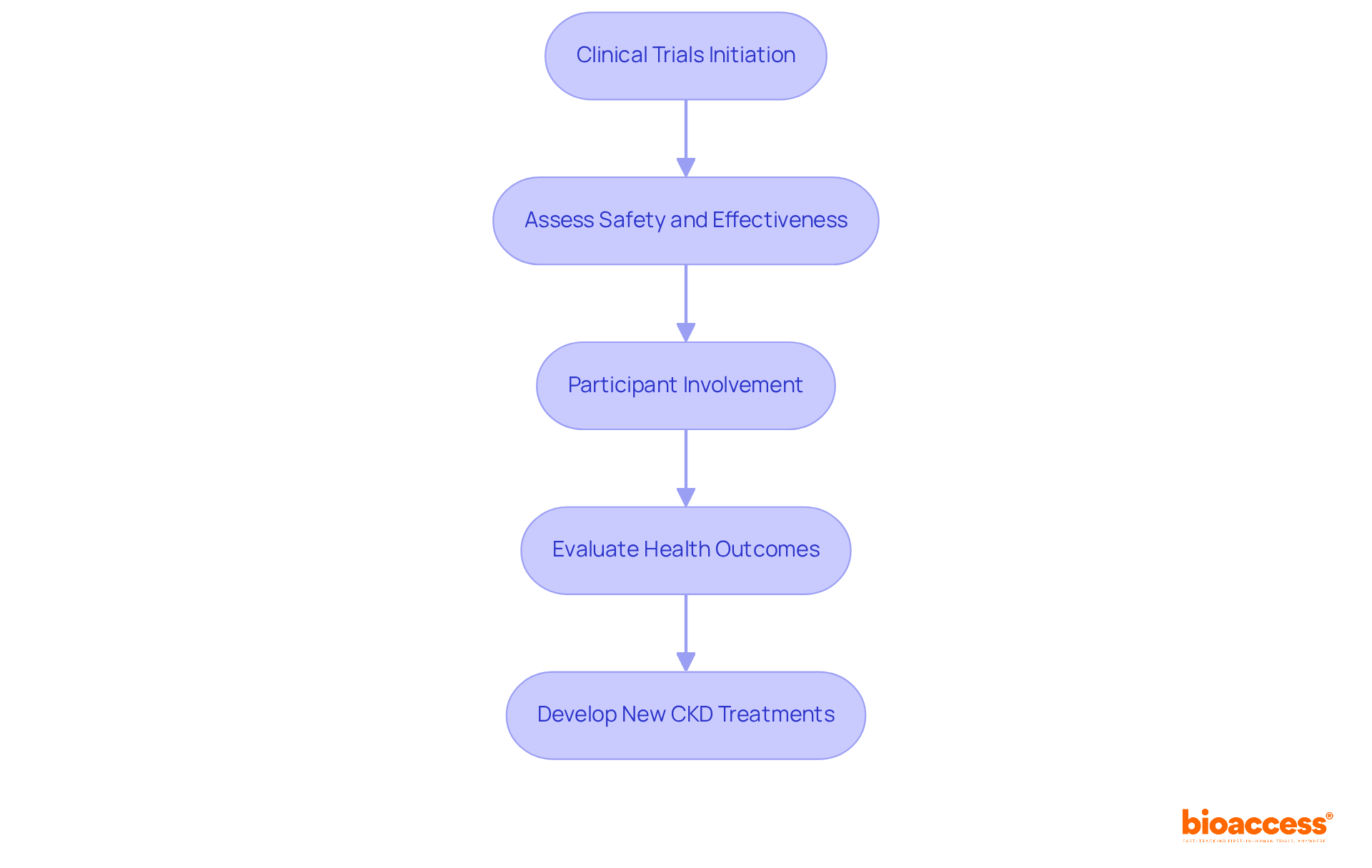
serve as the cornerstone for developing a , providing a . These studies not only enhance scientific understanding but also grant individuals access to . For example, recent trials have shown that participation can lead to , with some reporting a 25% reduction in cardiovascular and renal complications among participants. By , individuals play a crucial role in CKD research while potentially accessing a that may not yet be available commercially.
The rigorous methodologies employed in these trials ensure that the meets the highest standards of safety and effectiveness, ultimately leading to improved care for patients. As the prevalence of CKD continues to escalate, driven by factors such as an aging population and rising rates of type 2 diabetes, the necessity for becomes increasingly urgent. Recent initiatives, including the MoreTrials campaign, aim to streamline trial participation while prioritizing participant safety and reliable outcomes, thereby encouraging greater patient involvement in this essential area of research.
Conclusion
The advancements in chronic kidney disease (CKD) treatments highlighted in this article mark a pivotal shift towards more effective management strategies and innovative therapies for 2024. Collaborations with organizations like bioaccess®, the role of SGLT2 inhibitors, and the emergence of biomarkers such as cystatin C illustrate the rapidly evolving landscape of CKD care. These innovations promise not only to enhance patient outcomes but also signify a collective effort to tackle the complexities of CKD management.
Key insights reveal that strategies such as point-of-care testing, personalized risk assessments, and comprehensive lifestyle modifications are essential in delaying CKD progression. The exploration of new experimental treatments and the ongoing commitment to clinical trials further demonstrate a proactive approach in the fight against this prevalent condition. Each of these elements contributes to a nuanced understanding of CKD, enabling healthcare providers to tailor interventions that align with individual patient needs.
The significance of these developments cannot be overstated. As the prevalence of CKD continues to rise, it is crucial for healthcare professionals, patients, and stakeholders to stay informed and engaged with the latest advancements. Embracing these innovations fosters improved health outcomes and empowers individuals living with CKD to take charge of their health journey. The path forward is bright, and the commitment to research and collaboration will undoubtedly lead to a future where CKD management is more effective and accessible for all.
Frequently Asked Questions
What is bioaccess and what services does it provide for CKD treatments?
Bioaccess is a leading Contract Research Organization (CRO) in Latin America that specializes in accelerating clinical research services for chronic renal disease (CKD) treatments. It offers a comprehensive suite of services, including subject recruitment and trial data management, aimed at streamlining the clinical trial process and ensuring compliance.
How quickly can bioaccess achieve ethical approvals and activate clinical research sites?
Bioaccess can achieve ethical approvals in an impressive 4-6 weeks and activate clinical research sites in under 8 weeks.
What are Sodium-Glucose Cotransporter-2 (SGLT2) inhibitors, and how do they help in CKD management?
SGLT2 inhibitors are medications that prevent glucose reabsorption in the kidneys, enhancing glycemic control and alleviating renal workload. They have been shown to significantly slow CKD progression and reduce the risk of major adverse renal events and progression to CKD stage 5.
What are the benefits of SGLT2 inhibitors beyond glycemic control?
In addition to improving glycemic control, SGLT2 inhibitors offer cardiovascular benefits and lower the incidence of acute kidney injury (AKI).
What is Cystatin C, and why is it important in assessing renal function in CKD patients?
Cystatin C is a biomarker that is used to evaluate glomerular filtration rate (GFR) in CKD patients. It is less influenced by muscle mass compared to creatinine, making it a more reliable indicator of renal function, which allows for earlier detection of renal dysfunction and more accurate monitoring of CKD progression.
How is Cystatin C expected to impact CKD diagnostics?
As research continues to validate its effectiveness, Cystatin C is poised to become a standard in CKD diagnostics, enhancing personalized care strategies for patients.
List of Sources
- Sodium-Glucose Cotransporter-2 Inhibitors: Innovative Approach to CKD Management
- dmsjournal.biomedcentral.com (https://dmsjournal.biomedcentral.com/articles/10.1186/s13098-024-01547-x)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC12166609)
- nature.com (https://nature.com/articles/s41598-025-86172-y)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC11836049)
- dom-pubs.onlinelibrary.wiley.com (https://dom-pubs.onlinelibrary.wiley.com/doi/10.1111/dom.16569)
- Cystatin C: A Key Biomarker for GFR Assessment in CKD
- biorexdiagnostics.com (https://biorexdiagnostics.com/cystatin-c-a-biomarker-of-renal-dysfunction)
- mdpi.com (https://mdpi.com/1422-0067/25/15/8135)
- fortressdiagnostics.com (https://fortressdiagnostics.com/news/2023/march/renal-testing)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC7657956)
- pubmed.ncbi.nlm.nih.gov (https://pubmed.ncbi.nlm.nih.gov/32450046)
- Point-of-Care Testing: Enhancing CKD Management Through Immediate Results
- annalsofglobalhealth.org (https://annalsofglobalhealth.org/articles/10.5334/aogh.3884)
- medcitynews.com (https://medcitynews.com/2024/08/disrupting-trajectory-of-chronic-kidney-disease-mortality-rates-through-digital-health-platforms)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC11276233)
- diabetesjournals.org (https://diabetesjournals.org/care/article/44/9/2025/138877/Chronic-Kidney-Disease-Testing-Among-At-Risk)
- woodleytrialsolutions.com (https://woodleytrialsolutions.com/news/getting-straight-to-the-point-the-benefits-of-poct-in-chronic-kidney-disease-clinical-trials)
- Individual Risk Assessment: Tailoring CKD Treatments for Better Outcomes
- kidney.org (https://kidney.org/news-stories/10-inspiring-quotes-those-living-kidney-disease-part-two)
- 10 Inspiring Quotes for Those Living with Kidney Disease (https://kidney.org/news-stories/10-inspiring-quotes-those-living-kidney-disease)
- medicalxpress.com (https://medicalxpress.com/news/2025-08-current-diagnostic-tool-underestimates-kidney.html)
- trial.medpath.com (https://trial.medpath.com/news/0998721b8a3dcc87/roche-receives-ce-mark-for-first-ai-based-kidney-risk-assessment-tool)
- roche.com (https://roche.com/media/releases/med-cor-2025-10-06)
- Delaying CKD Progression: Strategies for Effective Management
- mdpi.com (https://mdpi.com/2072-6643/14/18/3787)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10205767)
- bmcnephrol.biomedcentral.com (https://bmcnephrol.biomedcentral.com/articles/10.1186/s12882-022-02745-3)
- academic.oup.com (https://academic.oup.com/ckj/advance-article/doi/10.1093/ckj/sfaf275/8250022)
- Hyperuricemia Management: Addressing a Common CKD Complication
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC11321800)
- sciencedirect.com (https://sciencedirect.com/science/article/pii/S2590059525000573)
- amjmed.com (https://amjmed.com/article/S0002-9343(15)01047-5/fulltext)
- evidence.nejm.org (https://evidence.nejm.org/doi/full/10.1056/EVIDoa2100028)
- mdpi.com (https://mdpi.com/1660-4601/18/2/387)
- Statin Use: Evaluating Benefits for CKD Patients
- acc.org (https://acc.org/Latest-in-Cardiology/Articles/2025/04/17/16/18/Statins-in-Patients-on-Dialysis)
- kidney.org (https://kidney.org/kidney-topics/statins)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC8901279)
- ajkdblog.org (https://ajkdblog.org/2025/06/18/statin-use-in-chronic-kidney-disease-an-interview)
- lipid.org (https://lipid.org/lipid-spin/potpourri-2015/statins-chronic-kidney-disease-and-dialysis-clinical-trials-mechanisms)
- New Experimental Treatments: Exploring Innovations in CKD Care
- 10 Inspiring Quotes for Those Living with Kidney Disease (https://kidney.org/news-stories/10-inspiring-quotes-those-living-kidney-disease)
- linkedin.com (https://linkedin.com/posts/national-kidney-foundation_10-inspiring-quotes-for-those-living-with-activity-7047281385845194752-mNZi)
- linkedin.com (https://linkedin.com/posts/national-kidney-foundation_10-inspiring-quotes-for-those-living-with-activity-7044744684778250240-nMSw)
- Clinical Trials: Paving the Way for New CKD Treatments
- kidneyfund.org (https://kidneyfund.org/treatments/clinical-trials-for-kidney-disease)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC7030944)

Leave a Reply