Introduction
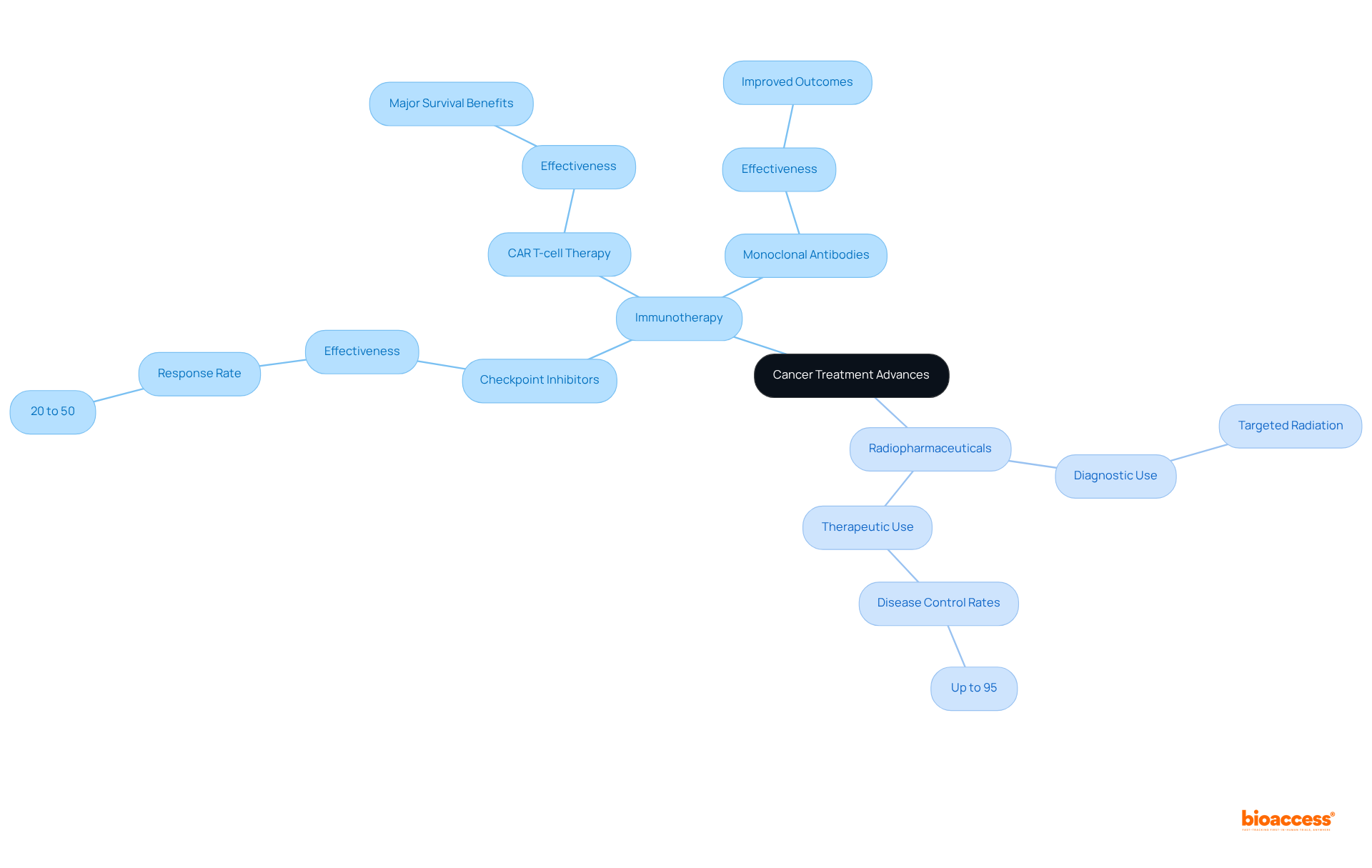
The landscape of cancer treatment is evolving rapidly, with innovative therapies such as immunotherapy and radiopharmaceuticals leading the charge against formidable tumors. These approaches not only offer unique mechanisms but also promise significant outcomes. However, their efficacy and safety profiles present a complex puzzle for oncologists and patients alike.
As the medical community delves deeper into the immunotherapy versus radiopharmaceuticals debate, critical questions arise:
- Which treatment truly offers the best hope for patients?
- How can these therapies be optimized to enhance survival rates while minimizing adverse effects?
Understanding Immunotherapy and Radiopharmaceuticals
harnesses the body’s immune system to combat tumors by enhancing its ability to identify and eliminate harmful cells. This innovative approach encompasses various modalities, including:
All of which have demonstrated significant promise in . For example, have revolutionized treatment for conditions such as melanoma and non-small cell lung cancer, exhibiting response rates ranging from 20% to 50%.
Conversely, for both diagnostic and therapeutic purposes, delivering targeted radiation directly to tumor cells. This method to surrounding healthy tissue, making it particularly effective for conditions like prostate and thyroid tumors. Recent studies indicate that can substantially enhance treatment efficacy, with certain therapies achieving as high as 95% in specific patient populations.
Both and represent critical advancements in oncology, making the vs comparison essential for instilling renewed hope for individuals facing challenging tumor diagnoses. As the field progresses, ongoing research is dedicated to exploring the potential of combining these therapies to maximize patient benefits.
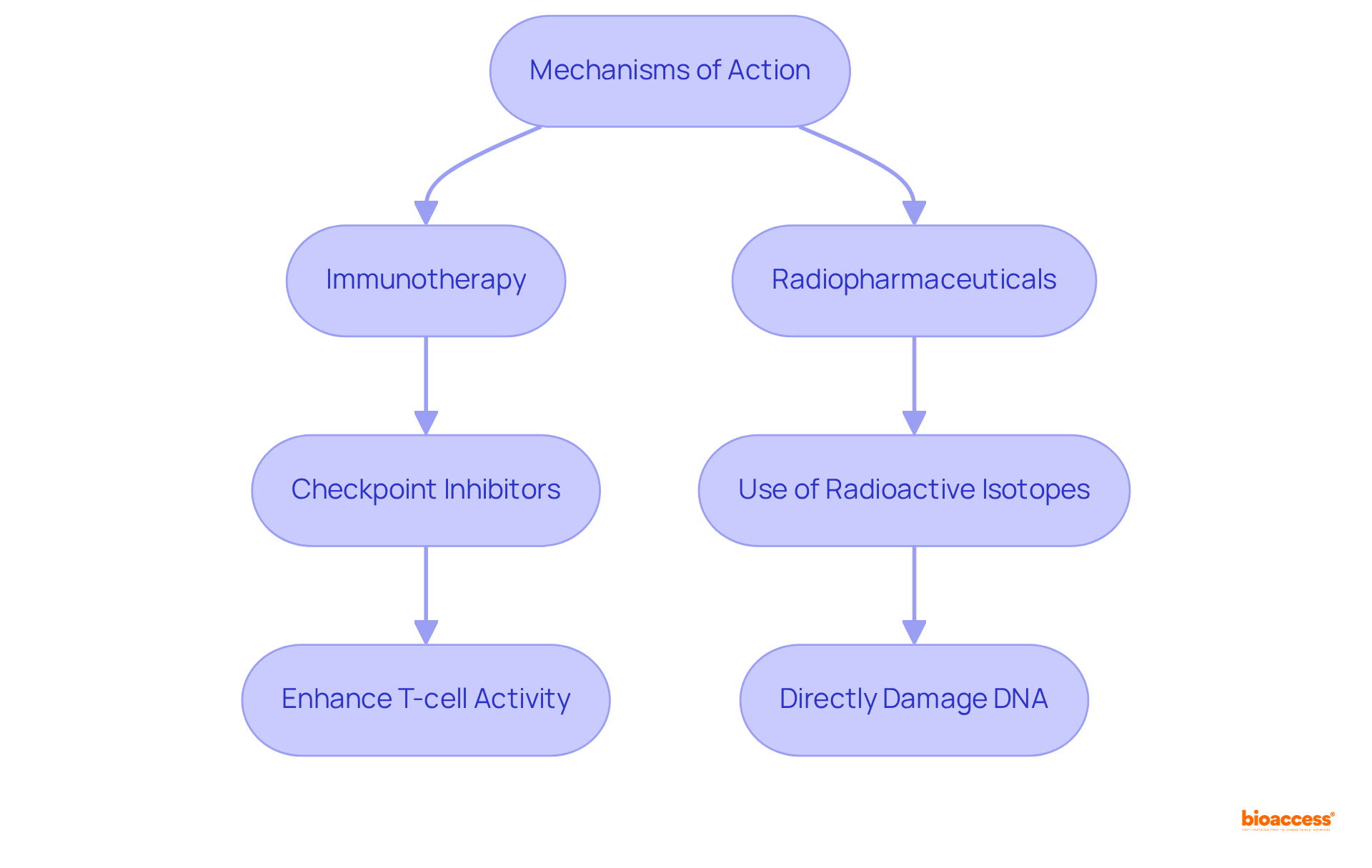
Mechanisms of Action: How Each Therapy Works
Immunotherapy plays a pivotal role in enhancing the . Notably, , thereby .
In contrast, the highlights that that emit radiation, directly damaging the DNA of malignant cells. This allows for the administration of while effectively sparing healthy tissues.
The interplay of these mechanisms holds the potential for , which can be further understood through an , thereby .
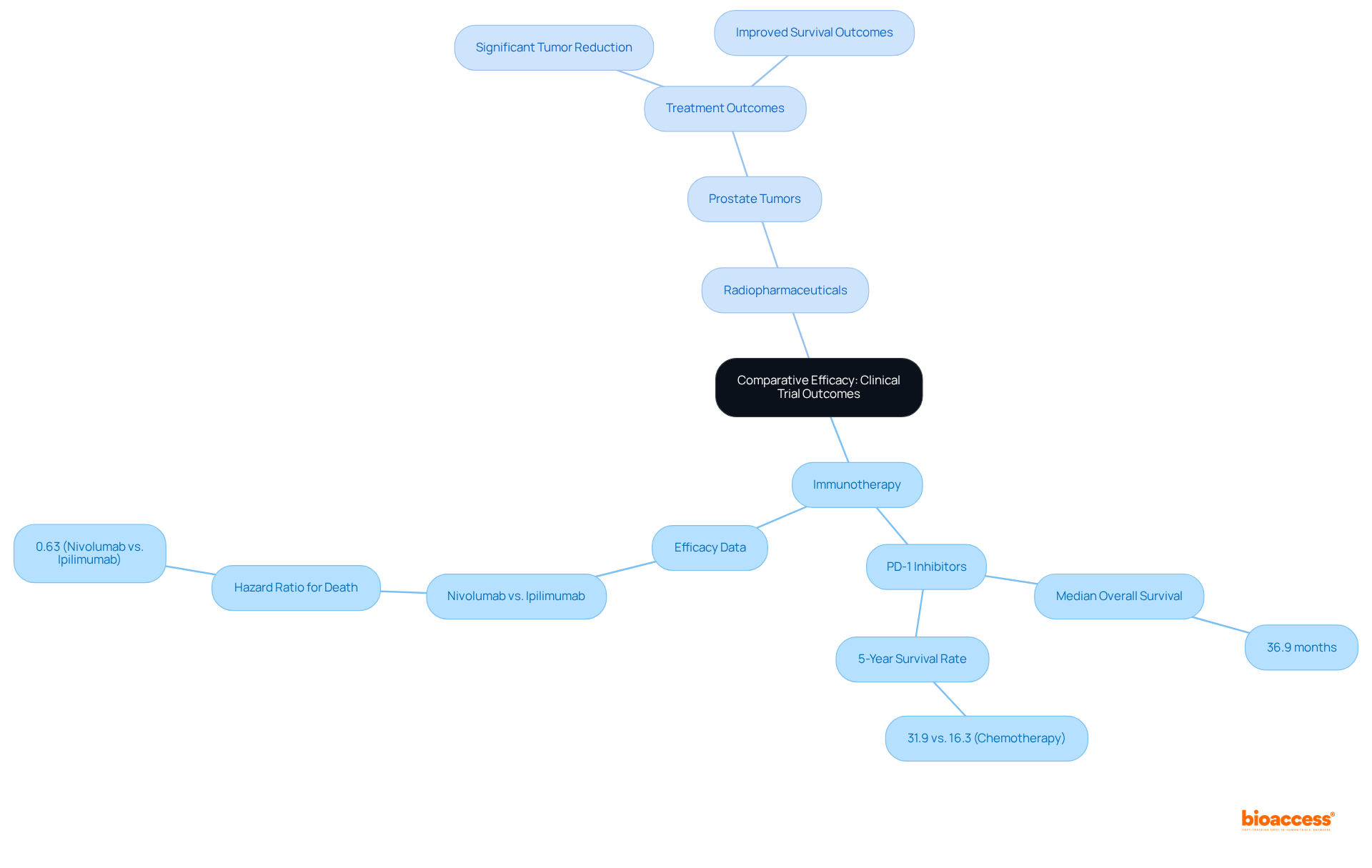
Comparative Efficacy: Clinical Trial Outcomes
have consistently demonstrated the efficacy of , particularly through PD-1 inhibitors, in yielding durable responses for conditions such as melanoma and lung tumors. For example, studies reveal that . In comparison, , with a notable 5-year overall survival rate of 31.9% versus 16.3% for chemotherapy.
Conversely, have proven to be effective treatments for specific tumors, particularly prostate tumors, where targeted radiation techniques have resulted in significant tumor reduction and improved survival outcomes. Nonetheless, the effectiveness of these therapeutic modalities, particularly in the , can vary markedly depending on tumor type and individual patient characteristics, emphasizing the critical need for a personalized approach to cancer treatment.
Moreover, the prevalence of the , present in approximately 40% to 50% of cases, underscores . It is equally important to consider the ; while chemotherapy often leads to hair loss and nausea, can result in immune-related side effects that require meticulous management.
A and their implications is vital for improving patient outcomes.
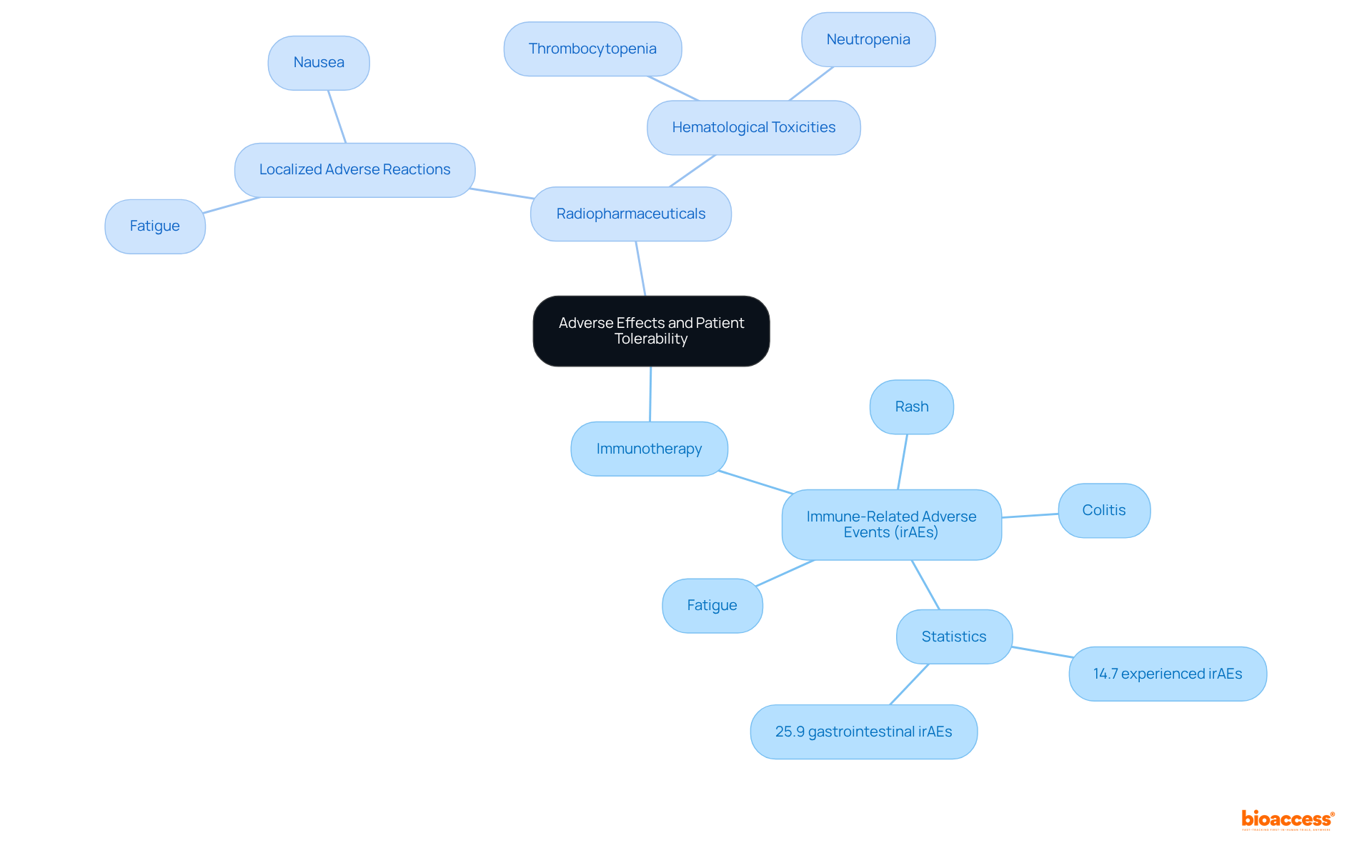
Safety Profiles: Adverse Effects and Patient Tolerability
The presents a critical area of focus due to the association of immunotherapy with (irAEs) that can affect multiple organ systems, including the skin, gastrointestinal tract, and endocrine system. Notable encompass:
- Fatigue
- Rash
- Colitis
With severe cases necessitating immunosuppressive treatments. A pivotal study revealed that 14.7% of individuals experienced irAEs 6 to 12 months after their initial exposure to (ICIs), underscoring the delayed nature of certain . In contrast, the shows that radiopharmaceuticals typically exhibit such as:
- Fatigue
- Nausea
Alongside potential like thrombocytopenia and neutropenia. The frequency of these varies, with fatigue reported by a substantial number of individuals undergoing both treatments. For example, among those treated with , 25.9% experienced , while the revealed hematological complications in a subset of patients receiving radiopharmaceuticals. The overall acceptability of these therapeutic approaches is contingent upon the patient, highlighting the importance of and throughout the care process. As oncologists emphasize, awareness of these potential side effects is crucial for optimizing patient outcomes and ensuring .
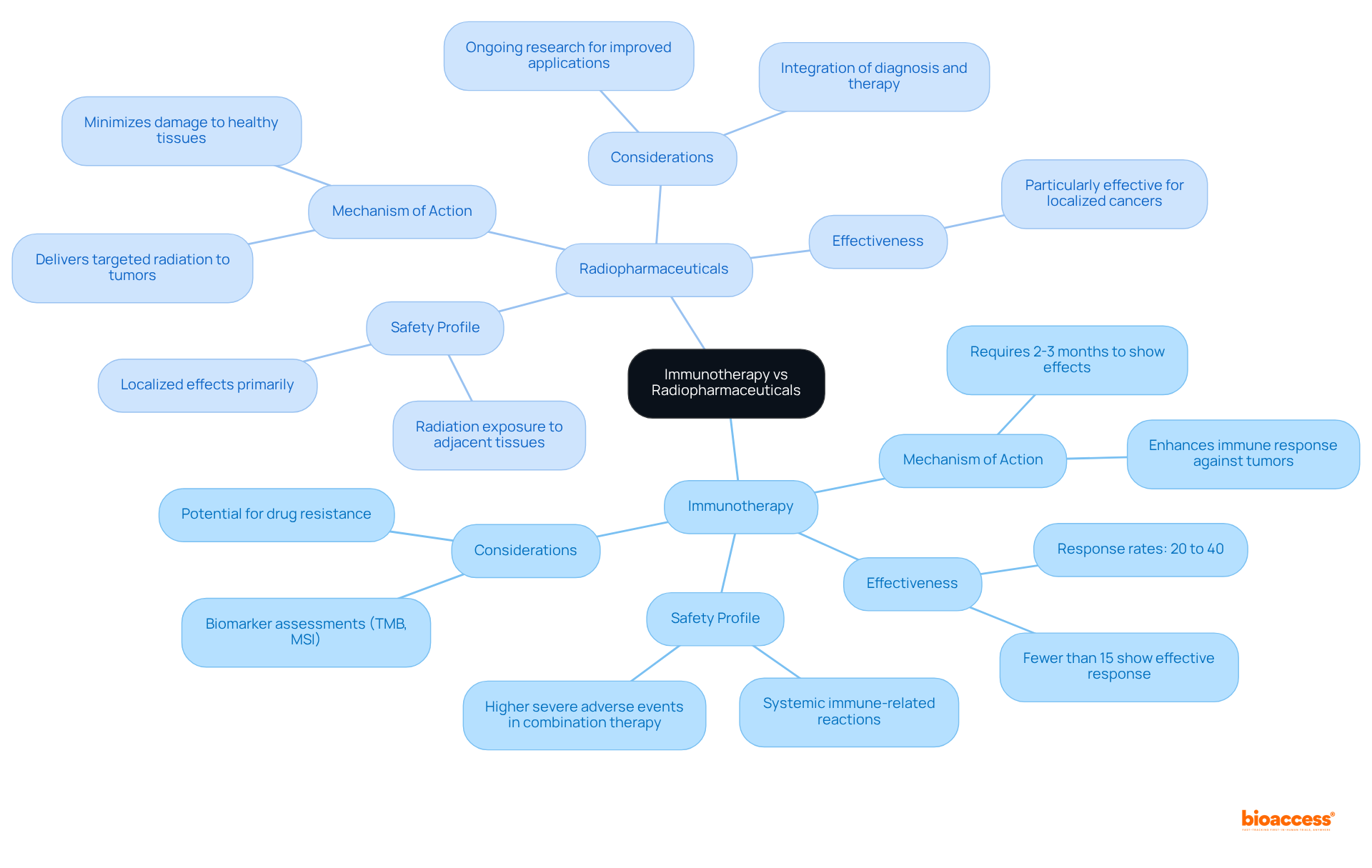
Key Differences and Similarities: A Summary
An highlights that both approaches represent innovative methods in oncology treatment, each functioning through distinct mechanisms.
- , often requiring 2 to 3 months to show effects on growths.
- The response rates for immunotherapy drugs vary, ranging from 20% to 40%, with fewer than 15% of patients exhibiting an effective anti-cancer immune response.
- In contrast, , proving particularly effective for .
The safety profiles of these modalities also diverge significantly.
- Immunotherapy is commonly linked to that can affect various organ systems, with increased occurrences of severe adverse events, such as pulmonary embolism and fever, particularly noted in combination therapy groups.
- On the other hand, typically result in localized effects, primarily involving radiation exposure to adjacent tissues.
Understanding these distinctions is crucial for healthcare professionals and patients as they and individual patient needs, particularly in the .
Moreover, , are essential in predicting responses to immunotherapy. As the field continues to evolve, ongoing research is dedicated to exploring the potential for combining these therapies to enhance overall treatment efficacy and safety.
Conclusion
Immunotherapy and radiopharmaceuticals signify pivotal advancements in cancer treatment, each utilizing distinct mechanisms to effectively target tumors. This comparative analysis emphasizes the critical need to comprehend the unique roles these therapies play in oncology and their potential to enhance patient outcomes in the ongoing battle against cancer.
The article delves into the mechanisms of action, efficacy, and safety profiles of both treatment modalities. Immunotherapy bolsters the immune system’s capacity to fight cancer, whereas radiopharmaceuticals deliver targeted radiation to tumor cells, thereby minimizing harm to adjacent healthy tissue. Clinical trial results indicate that both strategies can lead to significant improvements in survival rates, although their effectiveness is contingent upon tumor type and patient characteristics. Furthermore, the safety profiles reveal essential distinctions, with immunotherapy frequently leading to systemic immune-related adverse events and radiopharmaceuticals generally causing localized reactions.
As the landscape of cancer treatment evolves, it is imperative for healthcare professionals and patients to stay abreast of the latest research and advancements concerning immunotherapy and radiopharmaceuticals. A tailored approach, considering individual patient needs and specific cancer types, can optimize both treatment efficacy and safety. The ongoing investigation into the integration of these therapies holds promise for enhancing overall patient care and outcomes in the fight against cancer.
Frequently Asked Questions
What is immunotherapy and how does it work?
Immunotherapy is a treatment that harnesses the body’s immune system to combat tumors by enhancing its ability to identify and eliminate harmful cells. It includes various modalities such as checkpoint inhibitors, CAR T-cell therapy, and monoclonal antibodies.
What are some examples of immunotherapy modalities?
Examples of immunotherapy modalities include checkpoint inhibitors, CAR T-cell therapy, and monoclonal antibodies, all of which have shown promise in improving patient outcomes.
What types of cancer have benefited from checkpoint inhibitors?
Checkpoint inhibitors have revolutionized treatment for conditions such as melanoma and non-small cell lung cancer, with response rates ranging from 20% to 50%.
What are radiopharmaceuticals and how do they work?
Radiopharmaceuticals utilize radioactive substances for diagnostic and therapeutic purposes, delivering targeted radiation directly to tumor cells. This method minimizes damage to surrounding healthy tissue.
For which conditions are radiopharmaceuticals particularly effective?
Radiopharmaceuticals are particularly effective for conditions like prostate and thyroid tumors.
What is the potential efficacy of radiopharmaceuticals in treatment?
Recent studies indicate that certain radiopharmaceutical therapies can achieve disease control rates as high as 95% in specific patient populations.
Why is the comparison between immunotherapy and radiopharmaceuticals important?
The comparison between immunotherapy and radiopharmaceuticals is essential for instilling renewed hope for individuals facing challenging tumor diagnoses, as both represent critical advancements in oncology.
How do the mechanisms of action differ between immunotherapy and radiopharmaceuticals?
Immunotherapy enhances the immune system’s ability to recognize and eliminate malignant cells, while radiopharmaceuticals use radioactive isotopes to directly damage the DNA of malignant cells, allowing for high doses of radiation to tumors while sparing healthy tissues.
Is there ongoing research into combining immunotherapy and radiopharmaceuticals?
Yes, ongoing research is dedicated to exploring the potential of combining these therapies to maximize patient benefits and enhance overall treatment efficacy.
List of Sources
- Understanding Immunotherapy and Radiopharmaceuticals
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9592930)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC11027466)
- irbbarcelona.org (https://irbbarcelona.org/en/news/scientific/five-key-factors-predict-response-cancer-patients-immunotherapy)
- cancercenter.com (https://cancercenter.com/community/blog/2024/05/does-immunotherapy-work-for-everyone)
- cochiseoncology.com (https://cochiseoncology.com/what-is-the-success-rate-of-immunotherapy)
- Mechanisms of Action: How Each Therapy Works
- mdpi.com (https://mdpi.com/2072-6694/15/3/881)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC9139602)
- frontiersin.org (https://frontiersin.org/journals/medicine/articles/10.3389/fmed.2023.1192762/full)
- molecular-cancer.biomedcentral.com (https://molecular-cancer.biomedcentral.com/articles/10.1186/s12943-024-02212-7)
- cancer.org (https://cancer.org/cancer/managing-cancer/treatment-types/immunotherapy/immune-checkpoint-inhibitors.html)
- Comparative Efficacy: Clinical Trial Outcomes
- nejm.org (https://nejm.org/doi/full/10.1056/NEJMoa2407417)
- ncbi.nlm.nih.gov (https://ncbi.nlm.nih.gov/books/NBK470358)
- cancerresearch.org (https://cancerresearch.org/blog/difference-cancer-immunotherapy-and-chemotherapy)
- ascopubs.org (https://ascopubs.org/doi/10.1200/JCO.21.00174)
- ascopubs.org (https://ascopubs.org/doi/10.1200/JCO.21.01308)
- Safety Profiles: Adverse Effects and Patient Tolerability
- cancertreatmentreviews.com (https://cancertreatmentreviews.com/article/S0305-7372(24)00115-4/abstract)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC10247998)
- jamanetwork.com (https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2831992)
- pmc.ncbi.nlm.nih.gov (https://pmc.ncbi.nlm.nih.gov/articles/PMC5962379)
- jamanetwork.com (https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2814052)
- Key Differences and Similarities: A Summary
- cancer.gov (https://cancer.gov/news-events/cancer-currents-blog/2020/radiopharmaceuticals-cancer-radiation-therapy)
- cancercenter.com (https://cancercenter.com/community/blog/2024/05/does-immunotherapy-work-for-everyone)
- researchgate.net (https://researchgate.net/publication/383952745_Revolutionizing_cancer_treatment_The_role_of_radiopharmaceuticals_in_modern_cancer_therapy)
- nature.com (https://nature.com/articles/s41573-020-0073-9)

Leave a Reply